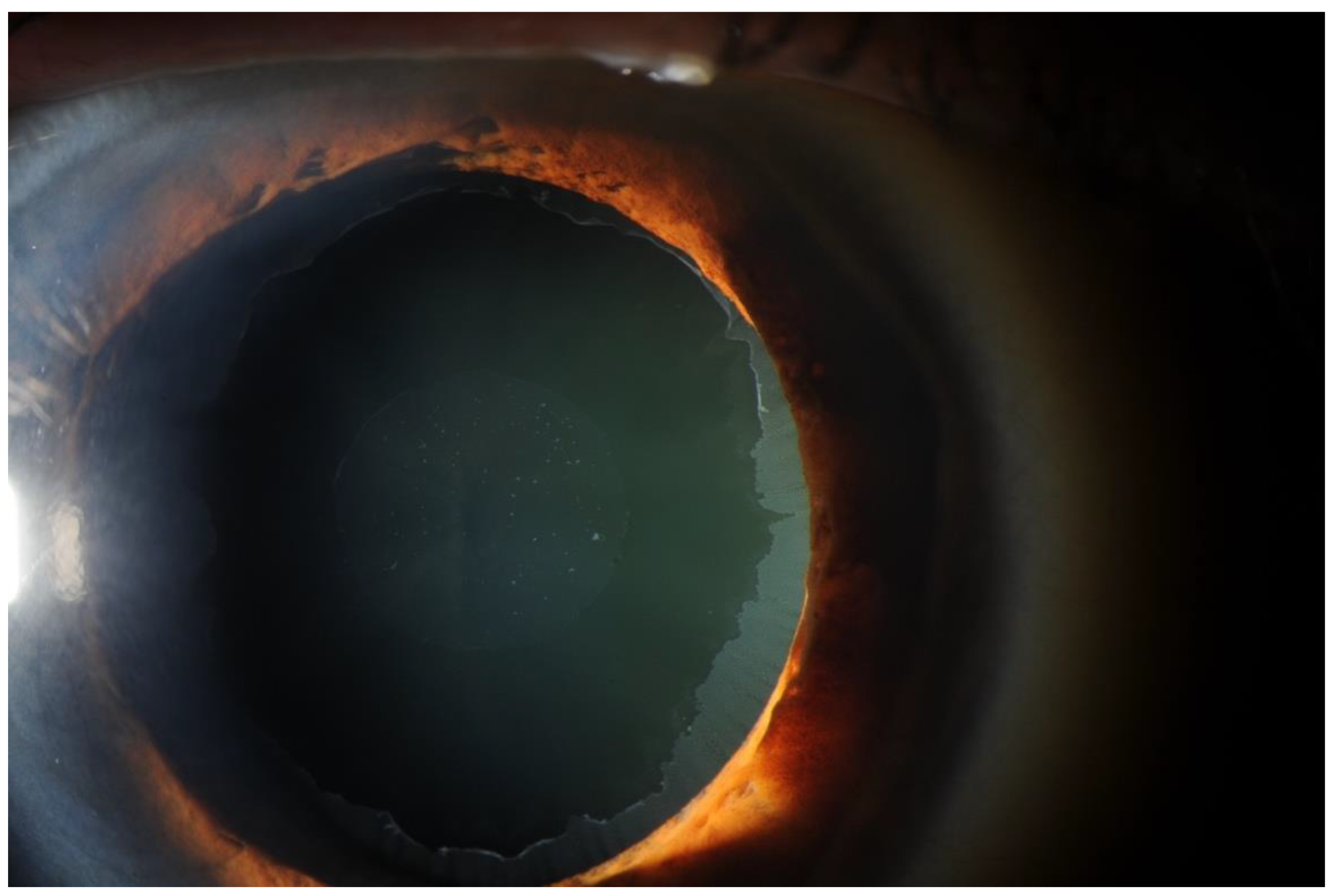
Pseudoexfoliation Syndrome
Title: Pseudoexfoliation Syndrome
Author: Chase Paulson. 4th year medical student at University of Utah
Photographer: James Gilman, CRA, FOPS
Overview: Exfoliation syndrome (XFS or PXF) is an age-related disease characterized by production and deposition of fibrillar extracellular matrix in systemic and ocular tissues. It was first described in 1917 by Dr. Lindberg in a Finnish population.1
XFS has been linked to various pathologies associated with extracellular matrix (ECM) dysregulation including inguinal hernia, pelvic organ prolapse, atrial fibrillation and chronic obstructive pulmonary disease.2-7
Pathophysiology: It is believed the fibrillin deposits in the anterior chamber impair aqueous humor outflow and precipitate more severe open angle glaucoma.8 XFS is bilateral but often presents asymmetrically (one eye is worse than the other) – the etiology of this is still poorly understood.
Further, patients often progress to exfoliation glaucoma (XFG), the most common identifiable cause of secondary open-angle glaucoma (OAG).9 When an individual with XFS develops signs of glaucoma (elevated IOP, visual field defects and thinning of the optic nerve), they are then classified as XFG. XFG progresses more rapidly than primary open-angle glaucoma with higher intraocular pressures (IOP), optic disc damage and the development of glaucomatous visual field defects.10 It is estimated that 40-60% of patients diagnosed with XFS will eventually develop glaucoma, based on prior multicenter studies.11,12 This is significant, as glaucoma is a leading cause of irreversible blindness worldwide.13
Risk factors: Although originally believed to be an inherited disease found primarily in Scandinavian descendants, the XFS phenotype has been reported in multiple populations and appears to be highly associated with genetic variants in the lysyl oxidase like-1 (LOXL1) locus, a key enzyme in ECM deposition and repair.
However, some individuals have the risk allele (LOXL1) and do not develop the disease, indicating environmental factors are likely at play. Elevated rates of XFS have been found in those with increased UV exposure and who live at latitudes further from the equator and at higher altitudes.14-17
PXF most commonly occurs in individuals above the age of 50.
Diagnosis
XFS is commonly diagnosed via dilated slit lamp examination with the identification of fibrillin deposits most commonly seen on the anterior lens capsule and at the iris margin. Iris transillumination defects are often noted. In a pseudophakic individual, gonioscopy should be performed to assess for pigmentary accumulation in the trabecular meshwork (TM) – as there will be no anterior lens capsule.
Symptoms
PXF is asymptomatic. XFG manifests with elevated IOP, visual field defects and thinning of the optic nerve all of which may remain asymptomatic until advanced stages of the disease.
Signs
The following signs can be explained by the pathogenesis of XFM depositing in various anatomical locations throughout the anterior chamber.
- Fibrillar XFM deposits in AC – including on anterior lens capsule, pupillary margin, corneal endothelium, and within the angle
- Hyperpigmented trabecular meshwork on gonioscopy
- Poor dilation
- Peri pupillary transillumination defects
- Phacodonesis (less common)18
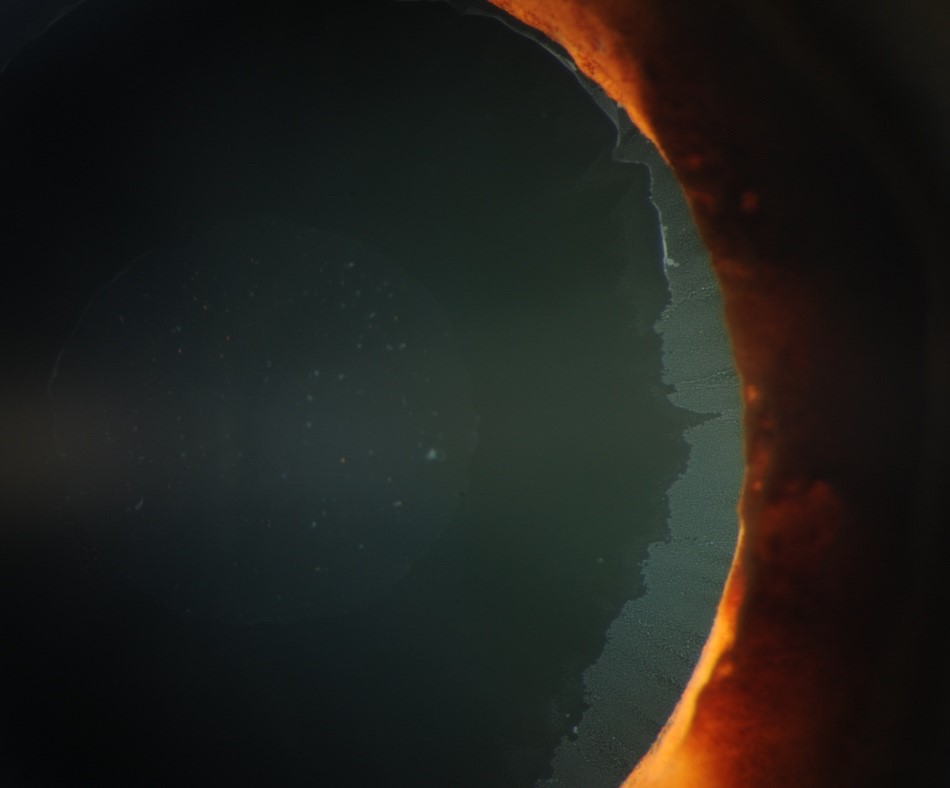
Figure 2. Pupillary border iris transillumination defect (lighter portion of iris) common in XFS. (19)
DDX
- Primary open angle glaucoma (POAG)
- True exfoliation syndrome
- Other causes of secondary OAG
- Pigment dispersion syndrome
- Iris neovascularization
Complications
- Development of XFG
- Special surgical consideration for cataracts
- Pre-operatively: lens subluxation, phacodonesis
- Intra-operatively: zonular weakness (from exfoliative material depositing in the zonules), drop nucleus
- Post-operatively: lens subluxation21
Management and treatment
Routine eye exams with monitoring for glaucoma – treat if warranted.
- Manage IOP to reduce glaucomatous progression
- If XFG, have closer follow-up than other OAG due to the unpredictability and rapid progression of glaucoma
- Have family members examined as there is some genetic component involved in the pathogenesis
References:
- Lindberg, J.G. Kliniska Undersokningar over Depigmenteringenav Pupillarranden Och Genomlysbarheten Av Iris Vid Fall Avaldersstarr Samt I Normala Ogon Hos Gamla Personer. In Clinical Studies of Depigmentation of The Pupillary Margin and Transilluminationof the Iris in Cases of Senile Cataract and Also in Normal Eyes in The Aged; Helsinki University: Helsinki, Finland, 1917.
- Bettis DI, Allingham RR & Wirostko BM (2014): Systemic diseases associated with exfoliation syndrome. Int Ophthalmol Clin 54: 15– 28.
- Besch BM, Curtin K, Ritch R, Allingham RR & Wirostko BM (2018): Association of exfoliation syndrome with risk of indirect inguinal hernia: the Utah project on exfoliation syndrome. JAMA Ophthalmol 136: 1368– 1374.
- Wirostko BM, Curtin K, Ritch R, Thomas S, Allen-Brady K, Smith KR, Hageman GS, Allingham RR. Risk for Exfoliation Syndrome in Women With Pelvic Organ Prolapse : A Utah Project on Exfoliation Syndrome (UPEXS) Study. JAMA Ophthalmol. 2016 Nov 1;134(11):1255-1262.
- Wirostko BM, Curtin K, Taylor SC, Paulson C, Pompoco C, Besch BM, Ranjan R, Ritch R. Risk of atrial fibrillation is increased in patients with exfoliation syndrome: the Utah project on exfoliation syndrome (UPEXS). Acta Ophthalmol. 2022 Jun;100(4):e1002-e1009. doi: 10.1111/aos.15017. Epub 2021 Sep 21.
- Shumway C, Curtin K, Taylor S, Sundar KM, Wirostko BM, Ritch R. Association between Obstructive Sleep Apnea and Exfoliation Syndrome: The Utah Project on Exfoliation Syndrome. Ophthalmol Glaucoma. 2021 May-Jun;4(3):260-267.
- Taylor SC, Bernhisel AA, Curtin K, Allingham RR, Ritch R, Wirostko BM. Association between Chronic Obstructive Pulmonary Disease and Exfoliation Syndrome: The Utah Project on Exfoliation Syndrome. Ophthalmol Glaucoma. 2019 Jan-Feb;2(1):3-10.
- Ozaki, M. Mechanisms of Glaucoma in Exfoliation Syndrome. J Glaucoma 27, S83 (2018).
- Ritch R. Exfoliation syndrome-the most common identifiable cause of open-angle glaucoma. J Glaucoma1994;3:176–7.
- Konstas AG, Jay JL, Marshall GE, Lee WR. Prevalence, diagnostic features, and response to trabeculectomy in exfoliation glaucoma. Ophthalmology. 1993;100(5):619-627. doi:10.1016/s0161-6420(93)31596-4
- Jeng SM, Karger RA, Hodge DO, Burke JP, Johnson DH, Good MS. The risk of glaucoma in pseudoexfoliation syndrome. J Glaucoma. 2007;16(1):117-121. doi:10.1097/01.ijg.0000243470.13343.8b
- Yamamoto T, Iwase A, Araie M, et al. The Tajimi Study Report 2: Prevalence of Primary Angle Closure and Secondary Glaucoma in a Japanese Population. Ophthalmology. 2005;112(10):1661-1669. doi:10.1016/j.ophtha.2005.05.012
- Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: the Right to Sight: an analysis for the Global Burden of Disease Study. Lancet Glob Health. 2020;9(2):e144-e160. doi:10.1016/S2214-109X(20)30489-7.
- Ye H, Jiang Y, Jing Q, Li D, Maimaiti T, Kasimu D, Lu Y. LOXL1 Hypermethylation in Pseudoexfoliation Syndrome in the Uighur Population. Invest Ophthalmol Vis Sci. 2015 Sep;56(10):5838-43.
- Pasquale LR, Jiwani AZ, Zehavi-Dorin T, et al.. Solar exposure and residential geographic history in relation to exfoliation syndrome in the United States and Israel.
- Stein JD, Pasquale LR, Talwar N, et al. Geographic and Climatic Factors Associated With Exfoliation Syndrome. Arch Ophthalmol.2011;129(8):1053–1060.
- Kozobolis, V.P.; Papatzanaki, M.; Vlachonikolis, I.G.; Pallikaris, I.G.; Tsambarlakis, I.G. Epidemiology of pseudoexfoliation in the island of Crete (Greece). Acta Ophthalmol. Scand. 1997, 75, 726–729
- https://eyewiki.aao.org/Pseudoexfoliation_Syndrome
- http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v3/v3c054b.html#ref
- https://webeye.ophth.uiowa.edu/eyeforum/cases/case8.htm
- Mohammed, S.; Kazmi, N. Subluxation of the lens and ocular hypertension in exfoliation syndrome. Pak. J. Ophthalmol. 1986, 2, 77–78.