Conjunctiva
Home / Ophthalmic Pathology / Conjunctiva
Macroscopic Overview – Normal Conjunctiva
Conjunctiva covers the surface of the globe (except cornea) and posterior eyelids. It is divided into bulbar, forniceal and palpebral sections. It also includes some unique zones such as the Plica Semilunaris. It contains many goblet cells, blood vessels, and immune cells.
- Bulbar Conjunctiva: covers visible surface of the globe (except cornea). Freely mobile, but does fuse with underlying Tenon’s Capsule.
- Palpebral Conjunctiva: covers posterior (inner) surface of eyelids. Not freely mobile. Many immune cells. The accessory lacrimal glands of Wolfring are located here.
- Forniceal Conjunctiva: located in fornices, forming a transition between the bulbar and palpebral conjunctiva. It is freely mobile and redundant to assist in eye movement. The accessory lacrimal glands of Kraus are located here.
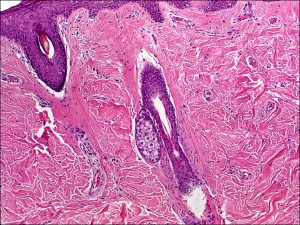
- Plica Semilunaris: located at nasal portion of conjunctiva. It forms a half moon like fold – contains many goblet cells, only portion of conjunctiva with sebaceous glands and hair follicles
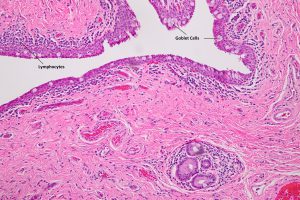
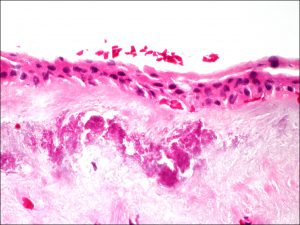
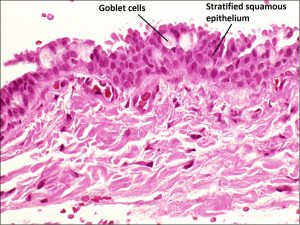
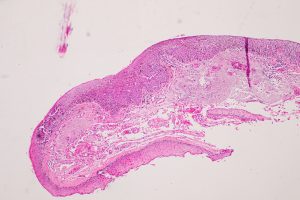
Nick’s Tips: The conjunctival surface is nonkeratinized, stratified squamous epithelium about 2-5 cells thick with goblet cells (generally very easily recognizable) present in normal and many pathological states. Look for the goblet cells in the epithelium and lack of keratin to distinguish from corneal epithelium and lids, respectively. By observing the key cellular features, the conjunctival should be easy to recognize. Remember, however, that there are some pathological states that may have a reduction in goblet cells or acanthosis (epithelial thickening), or may have surface keratinization (Examples: severe Sjogren’s, chemical burns, Stevens-Johnson disease, Ocular cicatricial pemphigoid, severe trachoma and severe ocular surface disease).
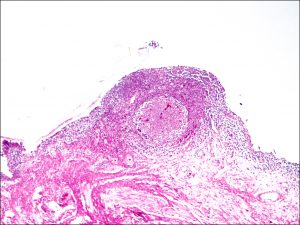
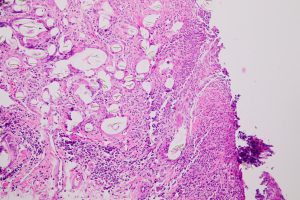
8.01 Low Magnification view of conjunctiva
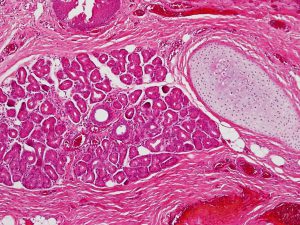
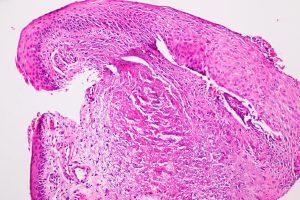
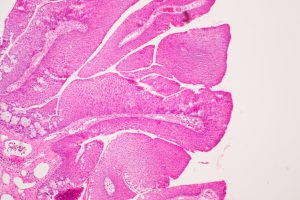
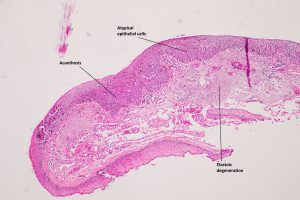
8.02 Medium magnification view of forniceal conjunctiva
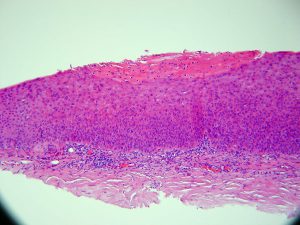
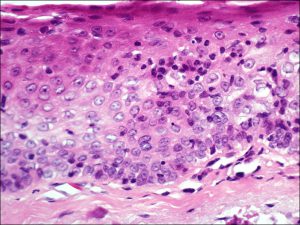
8.03 Higher magnification of forniceal conjunctiva
Limbal dermoid
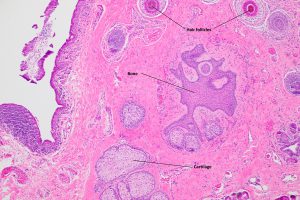
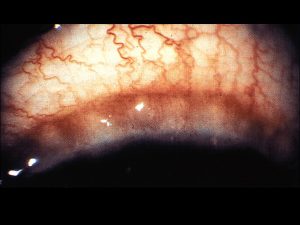
8.04 External Photo of limbal dermal choristoma
8.05 Limbal dermal choristoma
8.06 Limbal dermal choristoma
Nick’s Tips: epibulbar dermoids are a choristoma – benign collection of fully differentiated tissue located in an abnormal anatomic location (example: cartilage in the conjunctiva). Look for normal tissue elements in an abnormal location. Also look for syndromes such as Goldenhar Syndrome and Linear nevus sebaceous syndrome. Be careful if excising – the lesion may extend full thickness through the cornea – should have corneal graft available. Be careful – there are multiple structures in ocular pathology called dermoids.
Avoid confusion – Structures with dermoid in the name:
- Epibulbar limbal dermoid – solid (non-cystic) masses of connective tissue found at limbus)
- Complex choristoma – epibulbar limbal dermoid containing ectopic lacrimal gland or cartilage)
- Dermolipoma or lipodermoid – solid mass composed primarily of adipose tissue – usually superotemporal
- Dermoid Cyst – Orbital mass – lined internally with conjunctival epithelium. [link]
- Conjunctival dermoid – rare location of dermoid cyst – cystic structure lined internally with conjunctival epithelium. [link]
Epibulbar limbal dermoids
- Usually straddle the limbus
- Dome shaped white to yellow mass
- Often inferotemporal
- May have dermal structures or keratinized epithelium
- May extend full thickness through sclera or cornea
- Associated with the following syndromes (especially if bilateral)
- Goldenhar Syndrome: (oculoauriculovertebral dysgenesis) dermoid, eyelid coloboma, preauricular skin tag, vertebra deformities
- Linear nevus sebaceous syndrome: linear sebaceous nevus with brain and other systemic malformations, may be associated with genetic mosaicism.
Lipodermoid
8.07 Lipodermoid
- Usually superotemporal (in contrast to dermoid inferotemporal)
- Lipid component gives lipodermoid its name
- May extend posteriorly into orbit
- Also associated with Goldenhar and linear nevus sebaceous syndrome
Ectopic lacrimal gland
8.08 Lacrimal gland (plus cartilage) as conjunctiva
- Normal lacrimal gland located in abnormal location such as conjunctiva
Episcleral osseous choristoma
- Choristoma containing bone tissue in the conjunctiva
- Usually located superotemporally
Complex choristoma
8.09 Multiple choristoma types together in one lesion such as dermoid with bone.
Capillary hemangioma
Nick’s tips – look for many red blood cells in thin walled vessels in the substantia propria. Non-keratinized epithelium shows that this hemangioma is not located in lid or orbit.
- Look for red blood cells and many blood vessels proliferating in the substantia propria.
- Benign neoplasm vs hamartoma
- May involute without treatment
- Some reports of success using topical b-blocker (i.e. Timolol) as treatment.
Papillary conjunctivitis
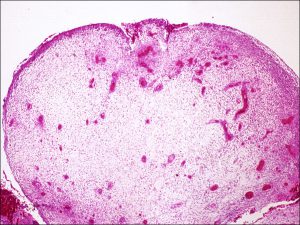
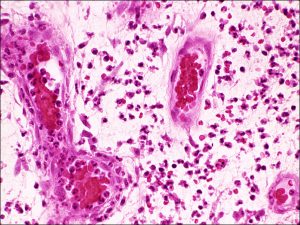
8.10 Central vascular core seen in papillary conjunctivitis
8.11 Central vascular core in papillary conjunctivitis
Nick’s Tips: note that the surface is flat with crypts. In higher magnification, look for cell types associated with allergy (eosinophils [link], plasma cells [link], mast cells [link]). Typically highly vascular with central blood vessel tuft.
- Papillary conjunctivitis – most commonly associated with allergic, vernal, atopic, or foreign body.
- Not pathognomonic for any particular type of conjunctivitis
- Papillae with central vascular cores, flat tops.
- Also will find eosinophils, lymphocytes, plasma cells and mast cells.
- When located at the limbus, papillae are called Horner-Trantas dots (associated with vernal keratoconjunctivitis)
Follicular conjunctivitis
8.12 Cobblestone appearance of follicular reaction
8.13 Follicle with lymphoid tissue and vessels around the edges
8.14 Large benign lymphocytes in a follicle
Nick’s Tips: follicles are clearer on their surface, papillae are redder on the surface. Follicles are usually avascular. Look for subepithelial germinal center consisting of a center of proliferating immature lymphocytes and a peripheral ring of plasma cells and mature lymphocytes.
- Follicular conjunctivitis – most commonly associated with viruses, atypical bacteria, toxins, and pharmaceuticals
- Small dome shaped nodule (sometimes described as tapioca appearing)
- Follicles most prominent in inferior palpebral conjunctiva and fornix.
- May be caused by reaction to glaucoma drops, especially brimonidine.
- Germinal centers are paler centrally with larger, immature lymphocytes and darker peripherally (the corona) with darker, mature lymphocytes and plasma cells.
Granulomatous conjunctivitis
8.15 Sarcoidosis
8.16 Foreign Body
Causes:
- Infectious: Parinaud Oculoglandular Syndrome [granulomatous conjunctivitis and preauricular lymphadenopathy] – Bartonella henselae (cat scratch), Francisella tularensis (rabbits), mycobacteria, syphilis
- Non-infectious: sarcoidosis – appears as small tan nodules – conjunctiva may be easier to biopsy than lungs, so look for possible site to biopsy in sarcoidosis suspect. Sarcoidosis will have aggregates of epithelioid histiocytes with small lymphocytic cuff +/- giant cells. Sarcoidosis should have zero central necrosis.
- Trauma: foreign body can cause granulomatous inflammation – look for foreign body, history of trauma, and multinucleated giant cells.
Infectious conjunctivitis
Nick’s Tips: consider the appropriate stains for each type: Bacteria (gram stain), Chlamydia (Giemsa), Mycobacteria (Ziehl Nielssen stain – acid fast), Fungi (periodic acid Schiff (PAS), Gomori methenamine silver (GMS), Mycobacteria spores (modified trichrome stains), viruses (viruses are too small to be seen in light microscopy – can see results of virus or use PCR (polymerase chain reaction)).
- Bacterial – varies by age group and exposure – H. influenza, S. pneumoniae, also gonococcal, etc.…
- Atypical bacteria – chlamydia (obligate intracellular pathogen)
- Serotype A, B, C – associated with trachoma
- Serotypes D-K associated with inclusion conjunctivitis
- Consider Giemsa stain of conjunctival scraping to look for organisms
- Viral – commonly adenovirus and herpes viruses (zoster and simplex)
- Fungal – typically involves cornea as well, rarely just a fungal conjunctivitis
- Parasites
- Microsporidia – common in HIV/AIDS
- Rhinosporidium seeberi – found in India, Southeast Asia and Southeast USA – comes from exposure to stagnant water.
Conjunctival membranes in Conjunctivitis:
True Membranes – tightly adherent, bleed when peeled. Associated with:
- Stevens-Johnson Syndrome
- Neisseria gonorrhea
- b-hemolytic Streptococcus
- Corynebacterium diphtheriae
Pseudomembranes do not bleed when peeled. Associated with:
- Adenovirus 8 – epidemic keratoconjunctivitis (EKC)
- Adenovirus 3 – Pharyngoconjunctival fever (PCF)
- Other bacterial infections
- Chemical burns
Some special cases of conjunctivitis:
Trachoma – Infectious conjunctivitis caused by the atypical bacteria Chlamydia trachomatous. Uncommon in the USA, but a major cause of blindness historically and worldwide.
- Serotypes A, B, and C cause trachoma.
- Spread by poor hygiene, direct contact with secretions, and flies.
- Conjunctival smear shows lymphocytes and PMNs and Leber cells (macrophages filled with phagocytosed intracellular debris)
- Conjunctival epithelial cells contain basophilic inclusions of Halberstaedter and Prowazek.
- Chronic trachoma will develop lymphoid follicles in the superior tarsus, limbus and fornix. Degeneration of the chronic follicles leads to Herbert’s pits (saucer-like limbal depressions).
- In later stages, the follicular response is replaced by papillary hypertrophy
- Pannus of the cornea with vascular downgrowth destroying Bowman’s membrane is a late complication
- The Arlt line is a band of linear scar tissue on the palpebral conjunctiva along the upper tarsus – parallel to the lid margin.
- The late cicatricial stage results in lid scarring with entropion and trichiasis. Severe chronic conjunctivitis results in destruction of goblet cells and obstruction of the accessory lacrimal ducts resulting in severe ocular surface disease and dry eye. Combined these lead to severe corneal disease leading to corneal blindness.
Vernal Keratoconjunctivitis:
8.17 Limbal vernal conjunctivitis
- Bilateral chronic papillary conjunctivitis
- Associated with seasonal recurrences typically in spring
- Frequently adolescent males
- May be worse in patients of African ancestry
- Large “cobblestone” papillae. Numerous eosinophils.
- Horner-Trantas dots (accumulated intra- and subepithelial collections of cellular debris and eosinophils located at the limbus)
- May have shield ulcer – superior corneal ulcer from abrasion of the cornea by the large palpebral papillae.
Giant Papillary Conjunctivitis
8.18 Giant Papillary Conjunctivitis
- Located on the superior palpebral conjunctiva
- Associated with long-term contact lens wear – either RGP or soft.
- Very large papillae and intense papillary reaction
Phlyctenular Conjunctivitis
- Classically associated with tuberculosis
- Most cases in USA related to staphylococcal blepharitis
- Characterized by inflammatory nodules on bulbar conjunctivitis near the limbus
- Overlying ulcerated epithelium.
Parinaud’s oculoglandular syndrome:
- Chronic granulomatous conjunctivitis cause by Bartonella henselae (cat scratch disease). Cat scratch does not usually occur on face or eye, but ocular symptoms are caused by spread via bacteremia.
- Stains poorly on gram stain.
- Stains well with Warthin-Starry silver stain.
- Conjunctival pathology shows many histiocytes with areas of focal necrosis.
Ligneous Conjunctivitis:
Nick’s Tips: Woody material is massive fibrin deposits – appears as granulomatous inflammation with sheets of very eosinophilic acellular material.
- Rare chronic pseudomembranous conjunctivitis
- Characterized by massive “woody” fibrin deposits.
- More common in children
- Pseudomembranes if removed tend to recur rapidly.
- Caused by mutation in plasminogen gene (autosomal recessive)
Ocular cicatricial pemphigoid
8.19 Ocular cicatricial pemphigoid
Nick’s Tips: Look for immunofluorescence specimens showing complement or immunoglobulins in the region of the basement membrane
- Autoimmune disorder attacking basement membrane that causes cicatricial scarring.
- Submit half of sample in Michel medium and half in formalin so that immunofluorescence studies can be done.
- 50% false negative on immunofluorescence, so absence does not rule out ocular cicatricial pemphigoid.
- Type II hypersensitivity reaction
- IgG antibodies against basement membrane components such as the beta- subunit of a6b4 integrin and laminin 5/epiligrin.
- Late OCP complications include severe lacrimal and Meibomian gland dysfunction epidermalization of the cornea and conjunctiva (keratin will be present) and severe or complete symblepharon.
Stevens-Johnson Syndrome / Erythema Multiforme
- Type III hypersensitivity
- Circulating IgA complexes
- Marked bullae formation
Pemphigus Vulgaris
- Autoantibodies against desmoglein 3
- Symblepharon does not occur
Pyogenic granuloma
8.20 Pyogenic granuloma
8.21 Granulation tissue in pyogenic granuloma
8.22 Pyogenic granuloma
Nick’s Tips: look for spoke like pattern of blood vessels and history of surgical or accidental trauma or chalazion. Not a true “pyogenic granuloma” as defined by dermatologist, but more accurately described as exuberant granulation tissue.
- Acute and chronic inflammatory cells
- Occurs at site of prior trauma or surgery or chalazion or other chronic irritation.
- Pedunculated reddish mass on eye with “spoke-wheel” blood vessels.
- Neither a true granuloma nor a necrotic mass – although some chalazion associated granulomas may be associated with inflammatory giant cells from the previous chalazion.
Pinguecula
8.23 Pinguecula
Nick’s Tips: look for elastoic degeneration and basophilic changes.
- Small yellowish nodule on conjunctiva
- Actinic damage (sun damage)
- Elastoic degeneration on histology – collagen stains with Verhoeff van Gieson stain for elastic fibers.
- Elastic staining does not decrease even in the presence of elastase (because elastic fibers are not being stained, degenerated collagen fibers are being stained).
Pterygium
8.24 Pterygium – crosses the limbus
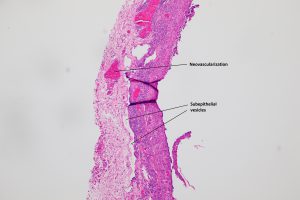
8.25 Pterygium, a subepithelial disease with solar elastosis, basophilic degeneration, and thinning of the epithelium
8.26 Calcium may be present in a pterygium
Nick’s Tips: look for elastoic degeneration – Verhoeff van Gieson stain will stain degenerated collagen. Look for basophilic degeneration.
- Epithelium may exhibit mild metaplasia and low potential for malignant transformation exists.
- Epithelium often thinned, but may be acanthotic (thickened)
- Stromal collagen shows basophilic degeneration and fragmentation.
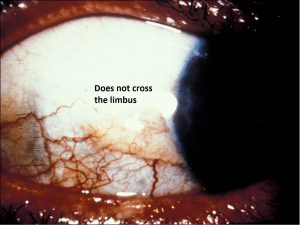
- Pterygium differs from pinguecula by location – extends onto the cornea.
- Pterygia show more prominent vasculature than pingueculae
- Pterygia may recur after excision (especially if not using a graft)
- Recurrent pterygia often do not show elastoic degeneration, but instead show prominent fibrovascular bundles and may extend through Bowman’s membrane.
- Recurrent pterygia may have p53 or p63 tumor suppressor mutations
Amyloidosis
8.27 Congo red staining in amyloidosis
Nick’s Tips: Apple green birefringence with polarized light and Congo red staining is a hallmark of amyloid. Can also stain with crystal violet or thioflavin T.
- Eosinophilic, relatively acellular hyaline material.
- Usually not associated with systemic amyloidosis
- Appears grossly as yellowish waxy nodules located on the epibulbar surface or diffusely infiltrating the substantia propria.
- Stains with Congo red. Birefringent on polarization microscopy.
- Amyloid composed of immunoglobulin light chains.
Epithelial inclusion cyst
8.28 Epithelial inclusion cyst may transilluminate on examination
8.29 Lining of epithelial inclusion cyst – goblet cells within the stratified squamous epithelium lining
- Lined by conjunctival epithelium
- Lumen appears empty or contains proteinaceous or mucinous fluid.
- Sometimes can calcify leading to calcific concretions in the conjunctiva – usually asymptomatic, but can rupture leading to foreign body sensation
Squamous papilloma
8.30 Squamous papilloma
Nick’s Tips: Must biopsy – cannot distinguish visually from papillomatous squamous cell carcinoma in situ or carcinoma – need histopathological diagnosis.
- Appearance of a fronds of conjunctival tissue with central vascular core.
- Usually caused by human papilloma virus (HPV)
- HPV6 – children – most commonly pedunculated in fornix, caruncle, margin. Often multiple and recurring.
- HPV16 – adult – usually flat, sessile, at limbus.
- Papillary fibrovascular fronds with acanthotic squamous tissue.
- Varying degrees of epithelial dysplasia cellular atypia and mitotic figures.
Ocular surface squamous neoplasia (OSSN)
Actinic keratosis:
8.31 Actinic keratosis with CIN with marked dysplasia
- Focal areas of leukoplakia
- Most frequently located on the surface of pingueculae or pterygia
- Focal acanthosis of the epithelium
- Surface parakeratosis overlying atypical epithelial cells
- Elastoic degeneration of the underlying substantia propria
Conjunctival Intraepithelial Neoplasia
8.32 Thickening is epithelial, not subepithelial in CIN
8.33 Thickening is epithelial, not subepithelial in CIN
8.34 Intact basement membrane seen in CIN
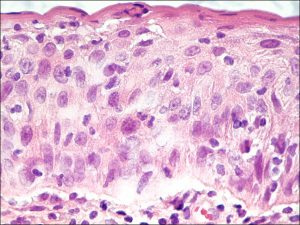
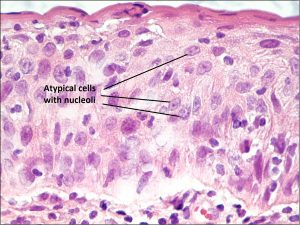
8.35 Severe CIN with nucleoli extending greater than 2/3 of the way through the epithelium
8.36 CIN with marked dysplasia
Nick’s Tips: Look for thickened epithelium (up to 10 X normal thickness), look for abnormal cells at the basal epithelium first. Abnormal cells may appear spindle shaped with very little epithelium or epidermoid with lots of eosinophilic cytoplasm. Mitotic figures may be common or extend to areas beyond the basal layer.
- Spectrum of disease
- Part or all of the epithelium replace by neoplastic cells
- CIN I- 0 to 1/3 of epithelium replaced
- CIN II- 1/3 to 2/3 of epithelium
- CIN III- 2/3 to almost entire epithelium
- Squamous Carcinoma in situ: involves entire epithelium but does not penetrate the epithelial basement membrane.
- Invasive squamous cell carcinoma: penetrates the epithelial basement membrane.
- May arise in areas in areas of solar elastosis
- May have white flaky surface (leukoplakia) – evidence of keratin production
- Often has thickened and gelatinous appearance.
- HPV 16 may be associated in areas without sun exposure.
- TX: excision with cryotherapy of margins topical mitomycin or interferon may be adjunct.
Squamous carcinoma in situ
- Carcinoma in situ- full thickness epithelium, BM intact
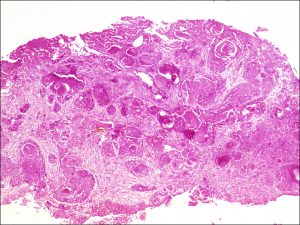
Invasive squamous cell carcinoma
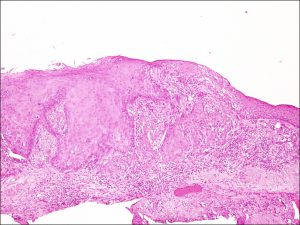
8.37 Squamous cell carcinoma is more likely to arise from the limbus than CIN
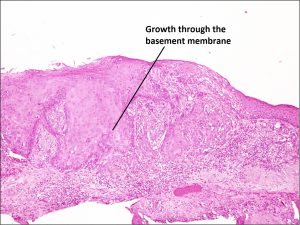
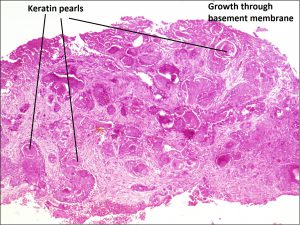
8.38 Disrupted basement membrane seen in SCC
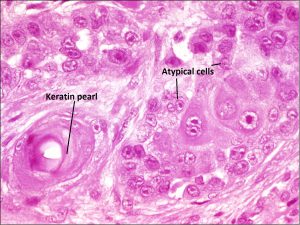
8.39 Invasive SCC with keratin pearls
8.40 Higher magnification of keratin pearls seen in SCC
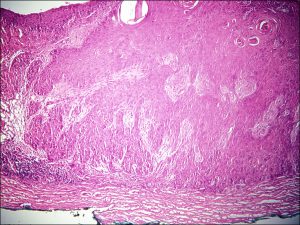
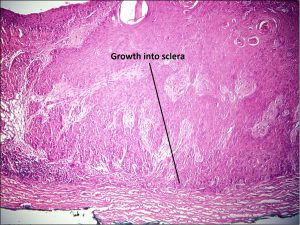
8.41 Invasive SCC growing into the sclera
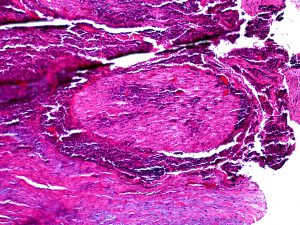
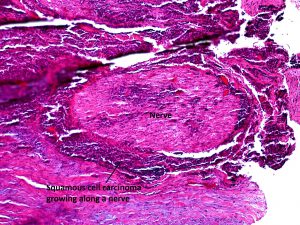
8.42 SCC can spread along a nerve to metastasize
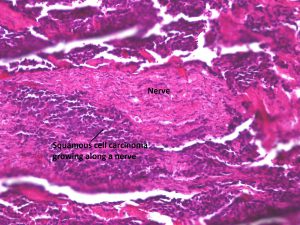
8.43 Another example of SCC growing along a nerve
- Invasive carcinoma- penetrates basement membrane.
- May extend onto cornea replacing corneal epithelium
- Is an uncommon sequelae of CIN/carcinoma in situ
- Epithelial cells may be sell- poorly differentiated cells in infiltrating nests in the stroma.
- Mucoepidermoid and spindle cell carcinoma (stains for cytokeratin on immunohistochemistry) are rare variants which are:
- more aggressive
- more likely to have intraocular spread
- May be more common or more aggressive in immunocompromised or HIV/AIDS
- Regional and systemic metastasis with death is possible, but very uncommon.
Hereditary Benign Intraepithelial Dyskeratosis (HBID)
- Rare-autosomal dominant
- Bilateral limbal conjunctiva plaques + oral lesions
- Starts in childhood, waxing and waning
- First seen in Haliwa-Saponi Native Americans in North Carolina
- Zero malignant changed reported.
Melanotic Lesions of the conjunctiva
Melanotic lesion Age begins Appearance Location Malignant potential
Freckle (ephelides) youth small conjunctiva zero
Racial melanosis youth diffuse conjunctiva zero
Benign acquired melanosis adult diffuse conjunctiva zero
Conjunctival Nevis youth small conjunctiva low
Ocular melanocytosis congenital diffuse sub-conjunctiva yes (uveal)
PAM middle age diffuse conjunctiva yes
Ephelides (freckles):
- Flat patches of increased pigmentation
- No atypical melanocytes or hyperplasia
- Increased pigmentation of the basal cell layer of the epithelium
Racial Melanosis:
- Flat patches of increased pigmentation
- May be extensive
- Occurs in people with dark skin pigmentation
- May occur at limbus
- Squamous epithelial cells contain melanin
- No atypical hyperplasia
Conjunctival nevus (multiple types)
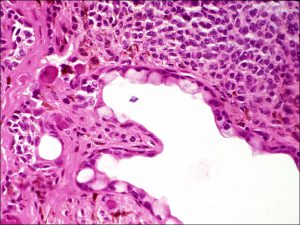
8.44 Nevus
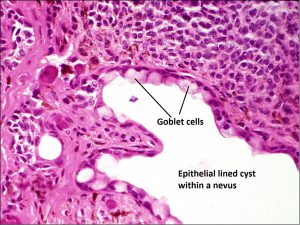
8.45 Epithelial lined cysts may be seen when removing a nevus, which indicates that the nevus has likely been present for years
8.46 Epithelial lined cysts may be seen when removing a nevus, which indicates that the nevus has likely been present for years
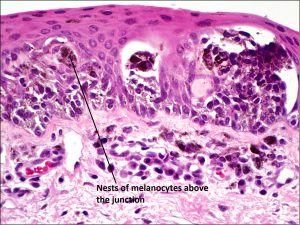
8.47 Junctional Nevus
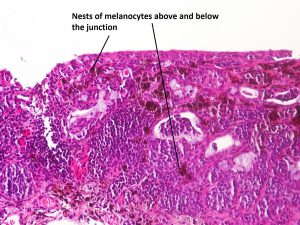
8.48 Compound nevus
8.49 Subepithelial (dermal in other areas of the body) nevus
Nick’s Tips: If nevus located in palpebral conjunctiva, then probably needs a biopsy as these are usually PAM or melanoma.
- Benign – most common conjunctival tumor in children
- Less than 1% evolve into melanoma
- Classified by location:
- Junctional: Nevus cells located at the epithelial-subepithelial junction – very rare in adults – should be considered PAM until proven otherwise if occurring in an adult.
- Subepithelial: nevus cells only in the conjunctival stroma. Most common in older adults.
- Compound Nevi: have both components – most common. May have cystic components of invaginated epithelium. May have minimal pigment or be amelanotic.
- Usually found in nests of nevus cells
- Hamartomatous
- Modified melanocytes
- Neural crest origin embryologically
- Nevi: early phase- nests of melanocytes near basement membrane
- Compound nevus – nests begin to drop off into substantia propria.
- Nevi are very rare in palpebral conjunctiva (usually PAM or melanoma)
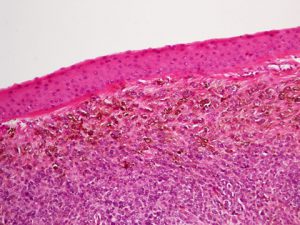
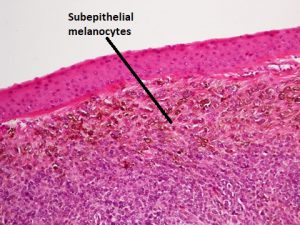
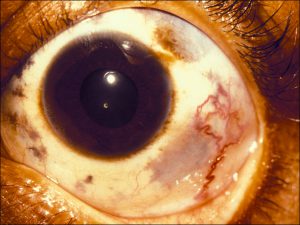
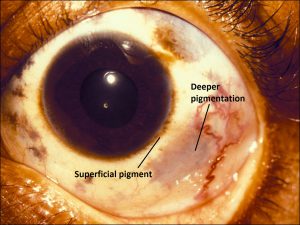
Nevus of Ota (congenital oculodermal melanocytosis or oculocutaneous melanosis):
8.50 Pigment seen superficially and deep to the sclera
Nick’s Tips: If unsure, anesthetize the eye and see if the pigmented lesion moves with the conjunctiva – if so, then the lesion is in the conjunctiva, not in the underlying tissue and therefore is one of the other melanocytic lesions, not oculodermal melanocytosis.
- Congenital melanocytosis of the epibulbar connective tissue and adjacent adnexal sin
- May have congenital hyperpigmented iris on side of lesion (heterochromia)
- Risk for melanoma of uvea, orbit, and CNS, but not increased risk of conjunctival melanoma.
- Pigment is not located in the conjunctiva, but rather in the deep epibulbar tissue, thus the conjunctiva will move freely over the lesion.
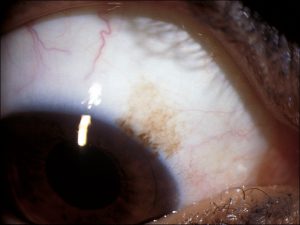
Primary acquired melanosis (PAM)
8.51 Superficial pigment in PAM without atypia
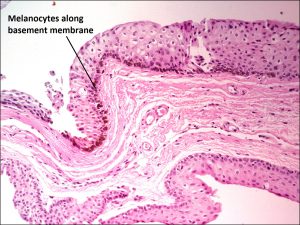
8.52 PAM without atypia – pigmented melanocytes seen along the basement membrane
8.53 Higher magnification view showing no atypia in this example of PAM
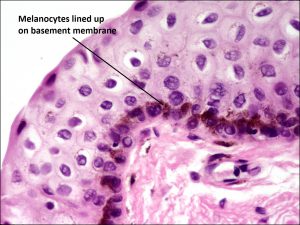
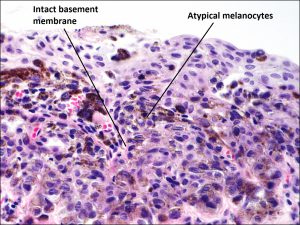
8.54 PAM with atypia – pigmentation may appear more substantial on exam
8.55 PAM with atypia – the melanocytes are contained within the basement membrane but have an atypical appearance.
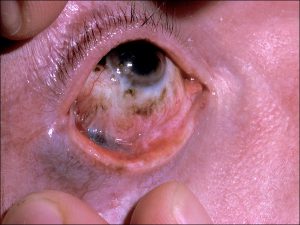
- PAM: unilateral flat patch of golden brown pigment with irregular margins
- May wax and wane or grow slowly.
- Usually occurs in middle-aged or elderly people
- Very rare in patients who have heavily pigmented skin – most common in white patients.
- Atypia must be evaluated in biopsy because of its influence on outcomes
- No atypia – no evidence of hyperplasia and pigment confined to conjunctival epithelial cells. Increased number of benign appearing melanocytes – very low risk of progression to melanoma
- Mild atypia – atypical melanocytes confined to basal layer of the epithelium – single cell lentiginous pattern. Low risk of progression to melanoma
- Severe atypia – atypical melanocytes escape basal layer or pagetoid or epitheliod appearance – very high risk of progression (up to 95%).
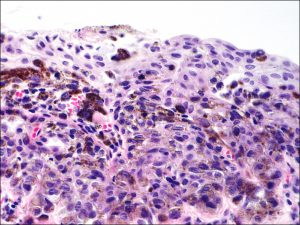
Conjunctival Melanoma
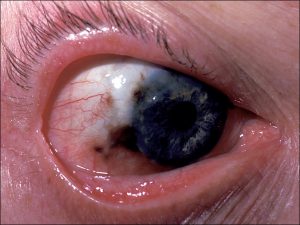
8.56 Scarring secondary to removal of PAM with atypia plus pigment seen in the fornix, which should be considered melanoma until proven otherwise
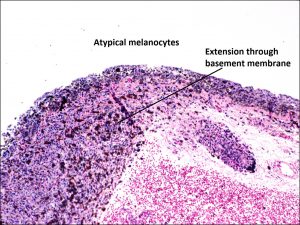
8.57 Melanocytes extending through the basement membrane in melanoma
8.58 Malignant melanoma secondary to PAM
8.59 Immunoperoxidase staining will indicate whether cells are melanocytes but not necessarily determine malignancy.
Nick’s Tips: Conjunctival melanoma more closely resembles skin melanoma than choroidal melanoma
- Atypical melanocytes spread through the conjunctival basement membrane – vertical growth of cells into the substantia propria.
- Malignant cells show nests (pagetoid) spread, epithelial migration or displacement.
- Pagetoid spread by epithelioid melanocytes **
- Full thickness replacement of epithelium ** (** most important predictors of invasion)
- Treatment:
- excise if small
- Cryotherapy for larger areas.
- Mitomycin C may be good treatment for larger diffuse areas of PAM
- 2/3 of conjunctiva melanomas arise from PAM with atypia.
- Aggressive lesions: beneath bulbar surface
- Mortality 25% – increased mortality if any of the following:
- thicker >1.8 mm
- Orbital or scleral invasion
- Pagetoid of full thickness intraepithelial spread.
- Eyelid skin involvement.
- Conjunctiva melanoma behaves more like skin melanoma than uveal melanoma.
- Stain for S-100, HMB-45 (most specific)
- TX: wide margin, no touch technique, alcohol epitheliectomy, cryo and radiation sentinel need biopsy (parotid/submandibular).
- Metastasis to lungs, liver, skin, brain.
Lymphoid tumors of the conjunctiva:
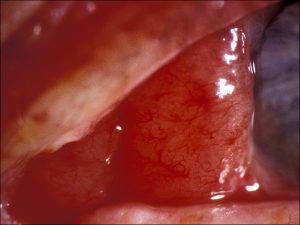
8.60 Conjunctival lymphoma is classically salmon colored on gross exam
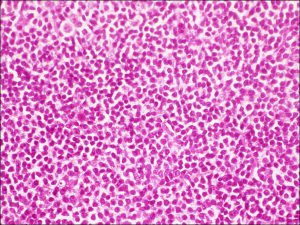
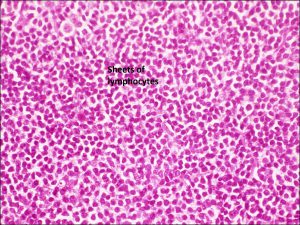
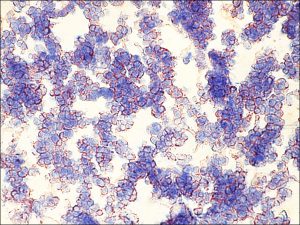
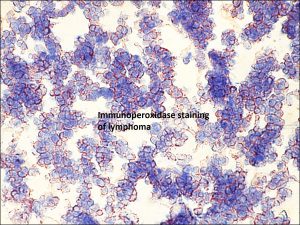
8.61 Sheets of lymphocytes seen in lymphoma
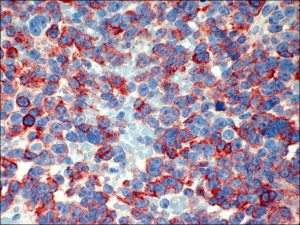
8.62 Immunoperoxidase stain of lymphoma. Typically these are of B-cell origin
Nick’s Tips: If suspect lymphoma, please send fresh specimen for flow cytometry analysis along with fixed specimen. Formaldehyde and paraffin processing destroy light chains and other markers.
- Range in a spectrum of disorders.
- Located in subepithelium / substantia propria.
- Salmon-colored patch, flat and smooth, intact overlying conjunctival epithelium
- Generally asymptomatic
- May need to rule out orbital involvement with imaging.
- Types:
- benign reactive lymphoid hyperplasia
- Mature, well differentiated lymphocytes in germinal centers.
- CD20+ B-cells in the follicular center and mantle zone.
- Low grade extranodal marginal zone lymphoma
- About half of ocular adnexal lymphoid lesions
- CD20 positive (B-cell marker) – do not stain for T-cell markers like CD3, CD5
- Generally excellent prognosis
- Systemic lymphoma present in about 20% of cases
- Systemic involvement more likely if bilateral or associated with adnexa and orbital tissue also present.
- benign reactive lymphoid hyperplasia
Oncocytoma
- Caruncule tissue is located at medial canthus – contains keratinized epithelium and adnexal appendages such as hair follicles and sebaceous glands. Lesions associated with skin and conjunctiva can be found at the caruncle.
- Oncocytoma may occur at caruncle