Ptosis
Home / Basic Ophthalmology Review / Lids/Lashes
Title: Ptosis
Author: Celestine Gregerson, MSIII University of Utah; Tom Dowdle, Matriculated Medical Student, University of Utah
Photographer: James Gilman, CRA, FOPS
Images:

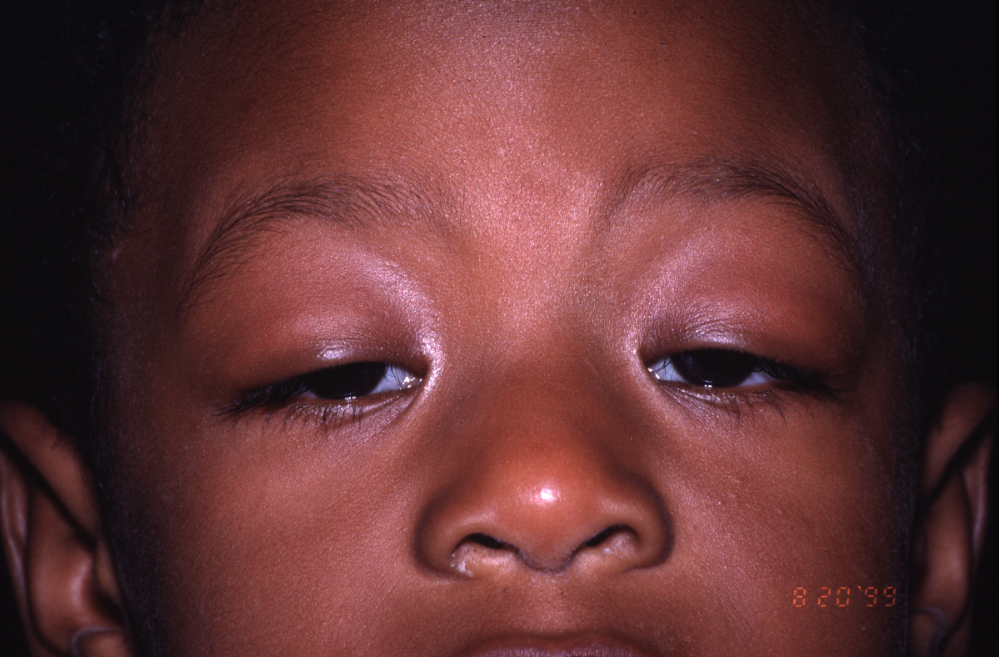
Figure 2: Asymmetric bilateral ptosis, more severe on the left. Obstruction of the pupil is present on both sides, resulting in significant bilateral visual field impairment
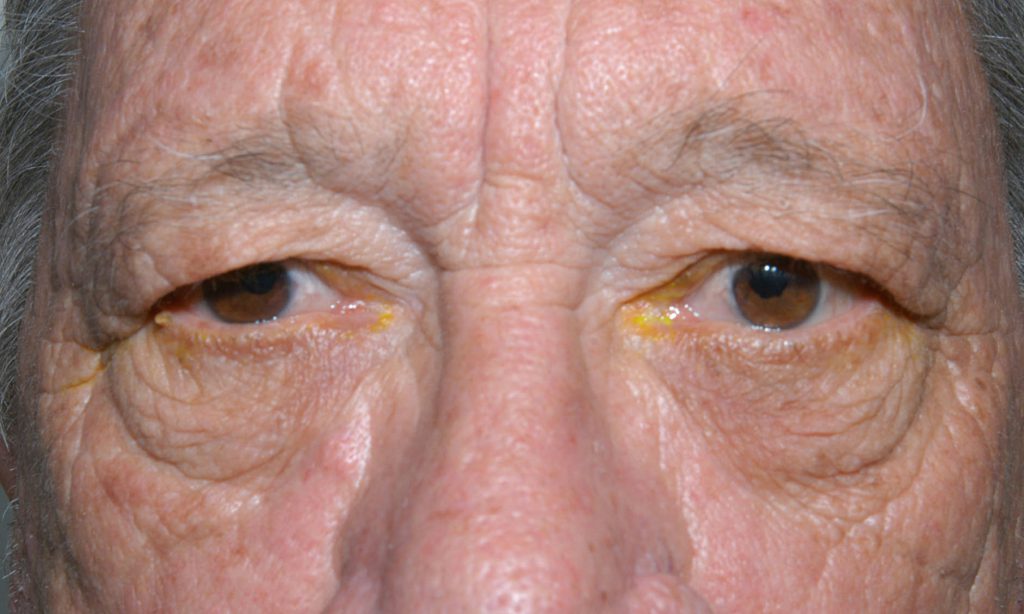
Figure 3: Dermatochalasis causing pseudoptosis, or drooping of the skin above the eyelids resulting in the appearance of ptosis.
Overview:
Blepharoptosis or ptosis refers to the drooping of the upper eyelid with an associated decrease in the vertical palpebral fissure, or the distance between the upper eyelid and lower eyelid.1,2 Ptosis occurs due to an abnormality in the structures that elevate the upper eyelid. In severe cases, ptosis can obstruct the pupil and cause visual field impairment. Etiologies include both congenital and acquired causes. Acquired causes include aponeurotic, neurogenic (the potentially emergent causes), and mechanical.
Classification & Etiology:
- Congenital: The most common cause of ptosis in children is due to the improper development of the levator palpebrae superioris muscle (levator), which functions to elevate the upper eyelid1,3. This is apparent on exam because there is no lid crease, which is where the levator normally inserts. Congenital ptosis is considered an emergency if the eyelid is obstructing vision because it can result in irreversible amblyopia or even vision loss if left untreated.
- Aponeurotic: The most common cause of ptosis in adults is due to weakening or disinsertion of the levator aponeurosis, the collagenous insertion of the levator on the eyelid. It may develop with aging, contact lens wear, chronic eyelid rubbing, or eye surgery.4-6 Aponeurotic ptosis typically is non-emergent and gradual in onset, but can cause significant upper visual field impairment.
- Neurogenic: Neurogenic ptosis is a potential emergency, especially when sudden onset. There are two especially concerning neurogenic causes: Horner’s syndrome and a cranial nerve III palsy. Myasthenia gravis is a less common cause of neurogenic ptosis.
- Horner’s Syndrome: This classically presents as a triad of findings due to disruption of the sympathetic innervation to the eye/face: ptosis, miosis (small pupil), and anhidrosis (absence of normal flushing/sweating). The ptosis is due to impaired innervation of the Müller’s or superior tarsal muscle, which is supplemental to the levator in elevating the eyelid. When sudden onset, it can be secondary to a carotid dissection, which warrants emergent referral to an Emergency Department for evaluation. In children, this can be secondary to a neuroblastoma compressing the sympathetic chain.
- Cranial Nerve III Palsy: Damage or disruption of this cranial nerve causes eyelid drooping because it innervates the levator. Typically, the ptosis is unilateral and the affected eye will present in a down-and-out position with a blown pupil1. The concerning etiology in these cases is an aneurysm or tumor compressing the nerve, and should be emergently referred for evaluation.
- Myasthenia Gravis: Fatigable unilateral or bilateral ptosis, as well diplopia or weakness of the orbicularis oculi often results from this autoimmune disorder. Ptosis seen in myasthenia gravis patients can be differentiated from other causes of ptosis by its temporary resolution with an ice-pack or an acetylcholine esterase inhibitor.1
- Mechanical/Traumatic Ptosis: Mechanical ptosis is a gravity-related drooping that occurs when there is edema, ecchymosis, or a mass of the upper eyelid that causes the lid to droop down. Trauma to the orbit can cause mechanical ptosis. However, trauma can also cause muscle or nerve damage resulting in persistent ptosis that does not resolve as local tissues heal.
- Other causes:
- Muscular disorders such as mitochondrial myopathies, myotonic dystrophy, and oculopharyngeal muscular dystrophy
- Neurotoxic causes such as botulinism or envenomation
Ptosis should not be confused with pseudoptosis, which is the perceived appearance of a dropping eyelid due to abnormalities of the globe or surrounding skin1. Pseudoptosis most commonly occurs as a result of dermatocholasis, the process in which the skin above the eyelid becomes less elastic and droops below the eyelashes7. Other causes of pseudoptosis include severe enophthalmos, ipsilateral hypotropia, brow ptosis, and contralateral lid retraction giving the impression of relative ptosis of the opposite lid.7
Evaluation:
Obtaining a thorough history, including any associated events or symptoms concerning for thyroid pathology or neurological abnormalities, is a first and critical step of ptosis evaluation7. The exam includes measuring:
- The function of the levator and superior tarsal muscles: how well the eyelid elevates when the patient is instructed to look up
- Comparing the distance between the eyelid and the center of the pupil between the two eyes in primary gaze
- Noting the presence or absence of an upper eyelid fold
- Noting any adaptations on the part of the patient:chin up posture or voluntary elevation of brows1,2,7
Management:
After the emergent causes of ptosis have been ruled out or addressed, candidacy for nonsurgical therapies in patients with myasthenia gravis or Horner syndrome can be considered. Eyelid crutches can be attached to eyeglasses for temporary relief in some patients. Surgery is the definitive corrective measure for patients with ptosis causing superior visual field loss.1,2,7 A variety of surgical approaches can be taken, including resection of the levator aponeurosis or eyelid suspension.2,7,8
Faculty Review: Griffin Jardine, MD
References:
- Patel K, Carballo S, Thompson L. Ptosis. Disease-a-Month (Clinical Issues in Ophthalmology – Part II). 2017; 63(3):74-79.
- Sudhaker P, Vu Q, Kosoko-Lasaki O, Palmer M. Upper eyelid ptosis revisited. American Journal of Clinical Medicine. 2009; 6 (3):5-14.
- Baldwin HC, Manners RM. Congenital Blepharoptosis: A Literature Review of the Histology of Levator Palpebrae Superioris Muscle. Ophthalmic Plastic and Reconstructive Surgery. 2002; 18 (4):301-307.
- Kersten RC, de Conciliis C, Kulwin DR. Acquired Ptosis in the Young and Middle-aged Adult Population. Ophthalmology. 1995; 102 (6):924-928.
- Mehat MS, Sood V, Madge S. Blepharoptosis Following Anterior Segment Surgery: a New Theory for an Old Problem. Orbit. 2012; 31 (4):274-278.
- Fujiwara T, Matsuo K, Kondoh S, Yuzuriha S. Etiology and Pathogenesis of Aponeurotic Blepharoptosis. Annals of Plastic Surgery. 2001; 46 (10):29-35.
- Fausett, BV, Nerad JA. Upper Eyelid Ptosis and Retraction. Diseases and Disorders of the Orbit and Ocular Adnexa. 2017; Ch 28: 525-539.
- Frueh BR, Musch DC, McDonald HMB. Efficacy and efficiency of a small-incision, minimal dissection procedure versus a traditional approach for correcting aponeurotic ptosis. Ophthalmology. 2004; 111(12):2158-2163.
Identifier: Moran_CORE_26610