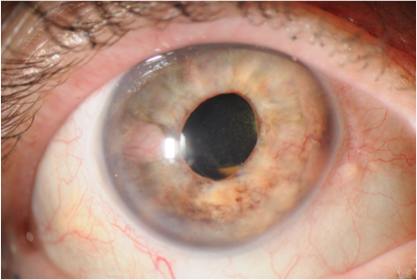
Iritis
Home / Basic Ophthalmology Review / Anterior Chamber
Title: Iritis
Author: Kristen Russell, MS4, Texas Tech University
Summary
Iritis is inflammation of the colored portion of the eye (Figure 1). Because the iris is one component of the uvea, it is also categorized as anterior uveitis. Iritis can be traumatic, infectious or autoimmune and can be localized to the eye or related to an underlying systemic disease. It is categorized by its presentation and course—unilateral versus bilateral, acute versus chronic, infectious versus non-infectious and granulomatous versus non-granulomatous.
Figure 1: Iritis with posterior synechiae
Presentation
Iritis can be asymptomatic, but most patients present with eye pain, photophobia, decreased vision, small or poorly reactive pupils and eye redness. Iritis is more commonly unilateral in which case the vision remains relatively normal in the affected eye. The key to diagnosis is seeing individual white blood cells (referred to as “cell”) and inflammatory proteins (“flare”) floating in the anterior chamber of the eye using a slit lamp magnified 16 times or 16X setting. Over the course of several days, these inflammatory cells can deposit on the cornea forming keratic precipitates (KP’s). (Figure 2) The underlying inflammation can also cause the iris to adhere to the lens (posterior synechiae) or the cornea (peripheral anterior synechiae). Often the inflammation will decrease aqueous secretion and increase uveoscleral outflow resulting in lower intraocular pressure (IOP). However, if inflammatory cells block the trabecular meshwork, the IOP could increase. Iritis that is chronic or reoccurring, may cause depositions of calcium on the front of the eye, known as band keratopathy.
Figure 2: Keratic Precipitates
Differential
The differential for patients presenting with iritis-like symptoms (pain, photophobia, poorly reactive pupils and eye redness) is broad, including but not limited to keratitis, conjunctivitis, acute angle closure glaucoma, endophthalmitis, scleritis and episcleritis. A careful history and slit lamp examination can differentiate between these conditions.
Workup
When a patient presents with iritis confirmed on slit lamp, systemic disease must be considered. Some of the infectious causes include Lyme’s disease, syphilis, toxoplasmosis, tuberculosis and HIV. Non-infectious or autoimmune causes include HLA-B27 related diseases (i.e. ankylosing spondylitis), juvenile idiopathic arthritis, Behcet’s disease, sarcoidosis and many more. The non-infectious causes respond to steroids but sometimes require steroid-sparing agents like other rheumatologic disorders. Before beginning these treatments, however, it is paramount to rule out the infectious causes. Therefore, a uveitis workup might include the following studies:
Lyme’s Disease: Anti-Borrelia burgdorferi antibodies
Syphilis: RPR, FT-ab
HLA-B27: HLA-B27 Genotype testing
Tuberculosis: Quantiferon Gold, Chest x-ray
Sarcoidosis: Chest x-ray, ACE
HIV: HIV-1, HIV-2 antibody screen
Behcet’s Disease: HLA-B51
Juvenile Arthritis: ANA
Treatment
Treatment of iritis involves trying to identify and treat an underlying cause (though many cases are idiopathic) while simultaneously decreasing the inflammation and minimize the discomfort and secondary damage to the eye from the inflammation. Once an underlying infectious cause has either been treated or ruled out, steroids are the primary therapy for decreasing inflammation—usually topical first but occasionally injectable or oral. Prompt management of the inflammation is important in preventing long term sequelae. Cyclopelegic agents or dilating eye drops such as atropine are also helpful in preventing iris adhesions from forming and reducing the pain and photophobia.
References:
Gutteridge IF, Hall AJ. Acute anterior uveitis in primary care. Clinical and Experimental Optometry. 2007. 90(2):70-82.
Leitman, Mark W. Manual for eye examination and diagnosis. Hoboken, NJ: John Wiley & Sons Inc., 2017. Print.
Identifier: Moran_CORE_24085
Copyright statement: Copyright 2017. Please see terms of use page for more information.