Eyelid Masses
Home / Basic Ophthalmology Review / Lids/Lashes
Title: Eyelid Masses
Author: Xavier Mortensen, MS4, University of Utah School of Medicine
LOCATION: Medical Student Education Outline > II. Anatomical Approach to Eye Disease > Lids/Lashes > 4. Masses
Eyelid Masses
Eyelid masses can be categorized into inflammatory, benign, or malignant masses. Below is a description of some of the more common masses found in each of these categories.
Inflammatory Masses
Chalazion
A chalazion is an inflammatory—but typically not infectious—mass of the eyelid that results from an obstruction of the Meibomian glands. It often presents with a dome-like elevation with surrounding erythema. The Meibomian glands are the oil-producing sebaceous glands on the posterior margin of the upper and lower eyelids. It can be associated with intense inflammation and therefore can be painful. If there is a superimposed bacterial infection, it may be purulent. It is commonly associated with rosacea and chronic blepharitis.
Treatment: Warm compress with gentle massage in addition to eyelid hygiene. Minocycline or doxycycline may be used for multiple and recurrent cases. It may take weeks to months to resolve fully.
Stye (External Hordeolum)
A stye is an acute infection of the sebaceous glands (glands of Zeis or Moll) of the anterior margin of the eyelid (often Staphylococcus aureus). It often appears to center around an eyelash follicle. It can be painful, hot, and swollen.
Treatment: Spontaneous resolution often occurs; however warm compresses and topical antibiotic ointment may be used if needed.
Benign Eyelid Lesions/Tumors
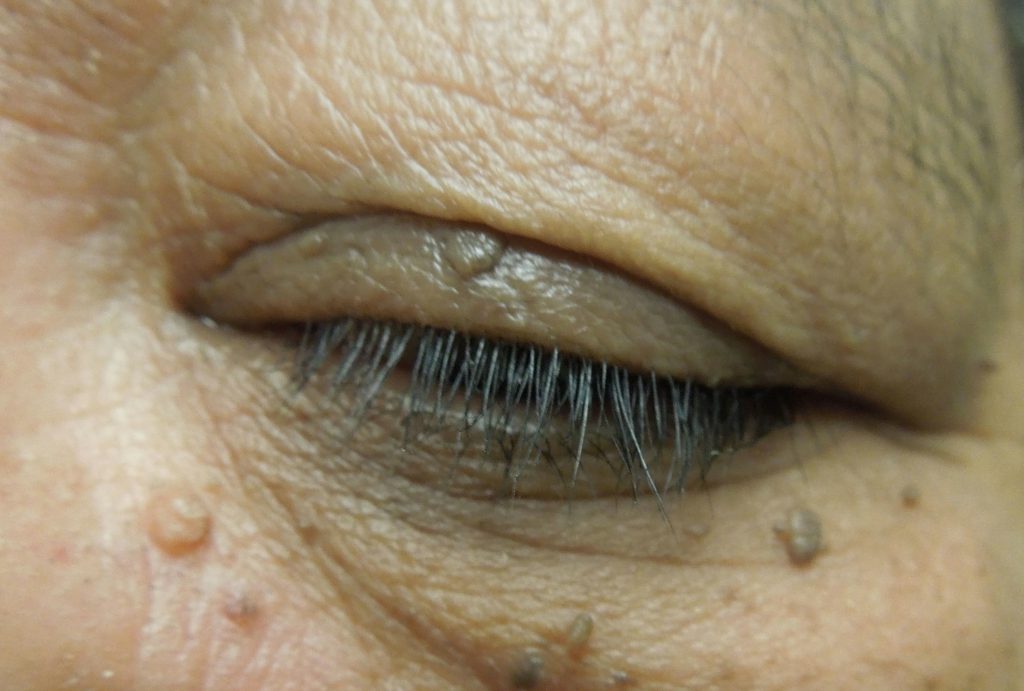
Squamous Papilloma
This is the most common benign eyelid tumor growth. The lesion is skin colored and can either be sessile or pedunculated. Pathology reveals epithelial hyperkeratosis and acanthosis around a central vascular core. It grows slowly and often forms groups of tumors in children, while in the elderly it more commonly is isolated as individual tumors or widely spaced tumors. The etiology isn’t completely understood, but increased age is a risk factor and may be associated with viruses in children.
Treatment: Complete excision
Verruca Vulgaris
This lesion is caused by infection by the human papillomavirus (often 6, 11, or 16). It presents as a pedunculated or sessile hyperemic mass on the eyelid with minimal surrounding inflammation. This lesion has potential for malignancy.
Treatment: Observe if small. Larger lesions can be excised, scraped, cauterized, or cryotherapy.
Moll’s Gland Cyst
This is caused by abnormal proliferation of moll’s gland. It appears smooth, translucent, and is slow growing and painless. It is more common in adults than children.
Treatment: marsupialization or complete excision
Malignant Eyelid Tumors
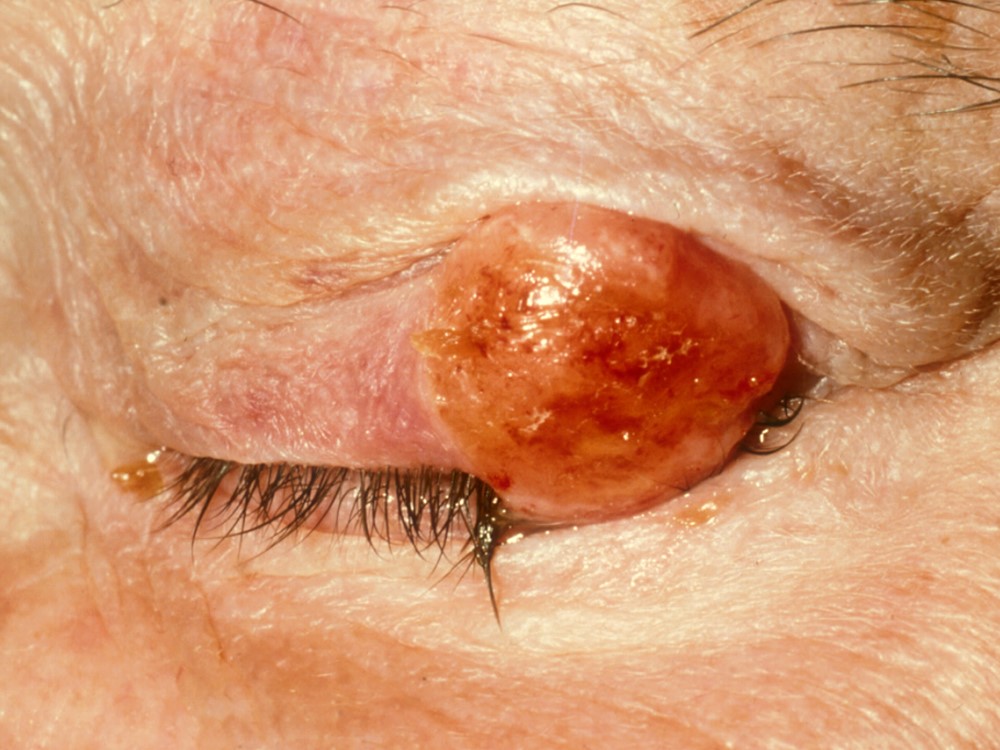
Basal Cell Carcinoma
This is the most common eyelid malignancy. It is most often found on lower eyelid and medial canthus region. Classic description: pearly border, telangiectasia, may ulcerate. Prolonged sun exposure, history of cigarette smoking, fair skin, are risk factors. It often presents in the middle-aged or elderly.
Treatment: Complete excision, Mohs surgery. Topical imiquimod. Protect against further sun damage.
Squamous Cell Carcinoma
This is much less common compared to basal cell carcinoma. Male gender, sun exposure, fair skin, immunosuppression, and radiation are risk factors. These present as a scaly, ulcerated, erythematous plaque that is most often found on the lower eyelid and lateral canthus region. It can be confused with basal cell carcinoma, but it usually does not have superficial vascularization, grows more rapidly, and hyperkeratosis is more frequent.
Treatment: Incisional or excisional biopsy. Adjunctive radiation, cryotherapy, or chemotherapy can be used as well. Protect against further sun damage.
Sebaceous Carcinoma
This is a highly malignant neoplasm that arises in the Meibomian or Zeiss glands. More common in older people (7th, 8th decade), females (2X as likely as males) and is more commonly found on the upper eyelid. It is often referred to as the “great masquerader” as it can present similarly to chronic blepharitis, recurrent chalazion, or basal or squamous cell carcinoma. These patients present with madarosis (eyelid loss), poliosis (skin or hair color de-pigmentation), and thick lid margin inflammation. Tumors can be yellow and hard. Lymphadenopathy is common.
Treatment: Wide surgical excision. Map biopsies of conjunctiva. Orbital exenteration is required in severe cases.
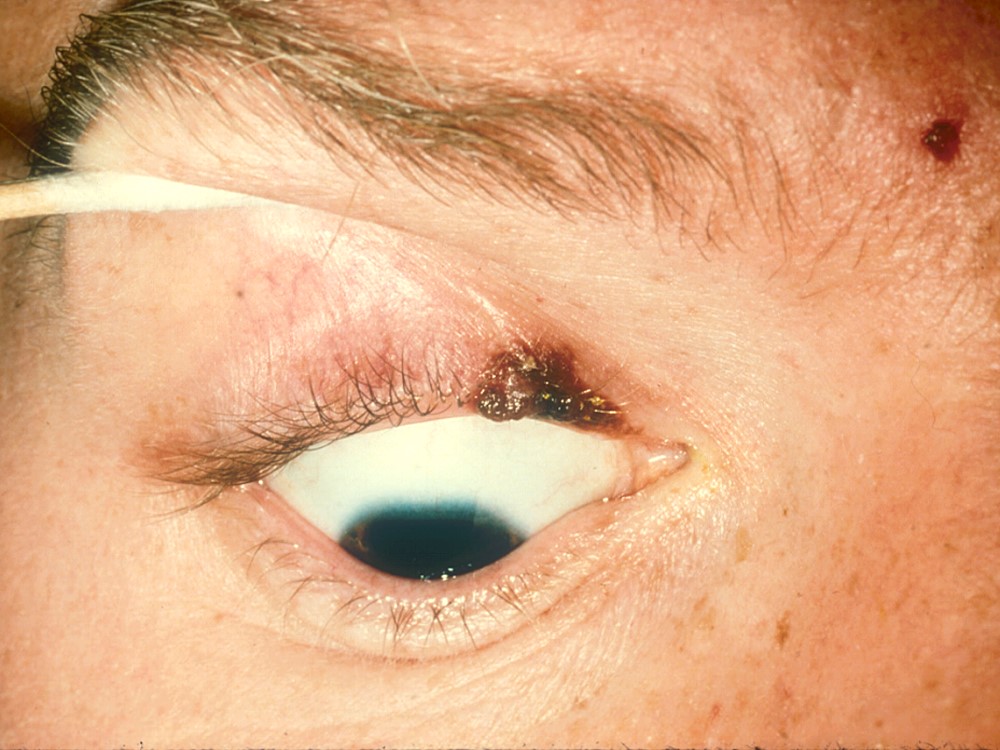
Malignant Melanoma
These often present as a dark, variable pigmented nodule or plaque with irregular, notched borders. Risk factors include sunlight exposure, genetic predisposition, and environmental mutagens. These are the most lethal primary skin tumors, but are rare (<1% of eyelid malignancies).
Treatment: Incisional or excisional biopsy or complete excision.
References:
- Bagheri, Nika, et al. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease. 7th Edition. Philidelphia: Wolters Klewer, 2017.
- Carreiro de Freitas, Ana Vega, Cat Nguyen Burkat and Simantha Khadka. Squamous Carcinoma of the Eyelid. 6 May 2016. 28 June 2018. <http://eyewiki.org/Squamous_Carcinoma_of_the_Eyelid>.
- Kaiser, Peter K, Neil J Friedman and Roberto Pineda. The Massachusetts Eye and Ear Infirmary Illustrated Manual of Ophthalmology. 4th Edition. Elsevier Inc., 2014.
- Skuta, Gregory L, Louis B Cantor and Jayne S Weiss. “Basic and Clinical Science Course.” Section 7: Orbit, Eyelids, and Lacrimal System. 2010-2011. American Academy of Ophthalmology, 2010. 164-166, 169-170, 181-190.
Photography Credit:
Chalazion, Squamous Papilloma: Douglas Marx, MD
Stye, Basal Cell Carcinoma, Sebaceous Carcinoma: Alison Crum, MD
Identifier: Moran_CORE_25570