Cataracts
Home / Basic Ophthalmology Review / Lens
Title: Cataracts
Author: Tanner Ferguson, 4th year medical student, University of South Dakota Sanford School of Medicine
IMAGES: Photography by James Gilman, CRA, FOPS, Moran Eye Center
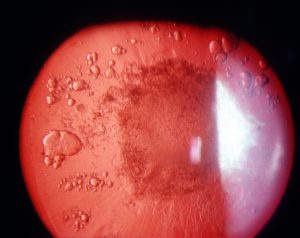
Figure 1: Retroillumination reveals a posterior subcaspular cataract centrally with vacuoles peripherally.
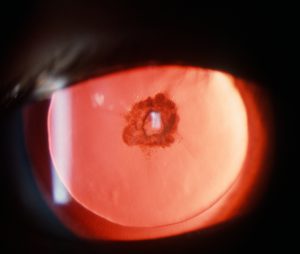
Figure 2: This central opacity would be visually significant due to its central location. Note the zonular fibers seen at the edge of the lens.

Figure 4: A slit lamp photo with a tangential beam of light highlighting a cross section of a more typical nuclear cataract with its accompanying yellowing.
Description:
Cataracts are an opacity or clouding of the crystalline lens in the eye1. Cataracts are extremely common and being able to recognize the common signs and symptoms is helpful for all clinicians. This introduction will provide a brief summary of the anatomy of the lens, risk factors for cataract formation and the symptoms associated with cataracts. For more detailed information of cataracts, please see our lens/cataract section of the CORE curriculum.
Anatomy
Normally, the human lens is a transparent, flexible biconcave disk that sits posterior to the iris (colored part of the eye) and is suspended circumferentially by zonular fibers from the ciliary body muscle. The lens is made up of three main parts: capsule, cortex and nucleus. The ciliary muscle contracts/relaxes to alter the shape of the lens to change its refractive power. This is particularly helpful for accommodation, or focusing on near objects, when contraction of the ciliary muscle changes the shape of the lens to bring near objects into focus. For more on accommodation, please see the Presbyopia topic (link).
Symptoms
The development and progression of cataract formation is dependent on numerous factors. Specific factors that can accelerate cataract formation include diabetes, steroids, trauma and intraocular surgery2,3. When cataracts do develop, patients may remain asymptomatic for some time. Symptoms typically differ depending on the type of cataract formation and its location within the lens. When they become visually significant, the common symptoms include difficulty driving at night, “starbursts” around lights, difference in color perception, cloudy vision or a change in eye glasses prescription4. Patients may even suggest their vision has improved, a phenomenon known as “second sight”, which occurs due to the change in refractive index of the lens with cataract formation5. Patients should be referred for cataract surgery when the cataract is affecting their visual needs.
Posterior Capsular Opacification
It’s also important to recognize a minor complication that many patients experience after cataract surgery. Although the capsule of the lens is typically polished and cleaned during cataract surgery, a small film can develop on the posterior capsule that is visually significant to patients, known as posterior capsular opacification (PCO). It can occur months to years after the initial procedure and is treated with an Nd:YAG laser capsulotomy, an office-based procedure.1,6 This is sometimes referred to as a “second cataract,” though this term is inaccurate as it is not a recurrence of the original cataract.
References:
- Olson RJ, Braga-Mele R, Chen SH, et al. Cataract in the Adult Eye Preferred Practice Pattern®. Ophthalmology. 2017;124(2):P1-P119. doi:10.1016/j.ophtha.2016.09.027.
- West SK, Valmadrid CT. Epidemiology of risk factors for age-related cataract. Survey of Ophthalmology. 1995;39(4):323-334.
- Klein BE, Klein R, Lee KE, Danforth LG. Drug use and five-year incidence of age-related cataracts: The Beaver Dam Eye Study. Ophthalmology. 2001;108(9):1670-1674.
- Crabtree HL, Hildreth AJ, O’Connell JE, Phelan PS, Allen D, Gray CS. Measuring visual symptoms in British cataract patients: the cataract symptom scale. British Journal of Ophthalmology. 1999;83(5):519-523.
- Brown NA. The morphology of cataract and visual performance. Eye (Lond). 1993;7 ( Pt 1)(1):63-67. doi:10.1038/eye.1993.14.
- Fong CS-U, Mitchell P, Rochtchina E, Cugati S, Hong T, Wang JJ. Three-year incidence and factors associated with posterior capsule opacification after cataract surgery: The Australian Prospective Cataract Surgery and Age-related Macular Degeneration Study. American Journal of Ophthalmology. 2014;157(1):171-179.e171. doi:10.1016/j.ajo.2013.08.016.
Identifier: Moran_CORE_24940
Copyright statement: Copyright 2018. Please see terms of use page for more information.



