Normal Eye Anatomy and Classification of Disorders
Home / Ophthalmic Pathology / Normal Eye
Normal Eye Anatomy Sections
- Whole Globe(includes vitreous section)
- Orbit
- Eyelid (with tear film)
- Conjunctiva
- Sclera
- Cornea
- Trabecular Meshwork
- Lens
- Iris
- Ciliary Body
- Choroid
- Retina
- Neurosensory Retina
- Retinal Pigment Epithelium
- Optic Nerve
Classification of disorders:
- Congenital
- Inflammation
- Degeneration and Dystrophy
- Neoplastic
- Infectious
Whole Globe
- Oblate spheroid with three main compartments
- Anterior chamber
- Between iris and cornea
- About 3mm deep and filled with around 200 µL of aqueous fluid
- Posterior Chamber
- Posterior to the iris and anterior to the lens and vitreous face
- Filled with around 60 µL of aqueous fluid
- Vitreous Cavity
- Comprises more than 2/3 of the eyes volume
- Anterior chamber
- Three layers
- Outer layer comprised of cornea (anteriorly) and sclera (posteriorly)
- Middle layer contains uvea –choroid, ciliary body, and iris
- Inner layer –retina
Orbit
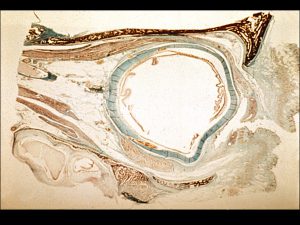
1.01 Sagittal section of the globe with surrounding orbital tissues
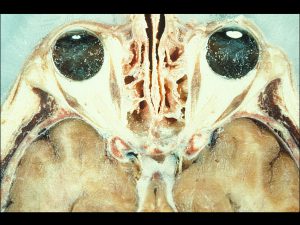
1.02 Axial cut of the orbit, both eyes.
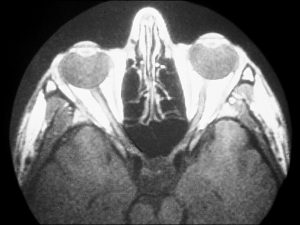
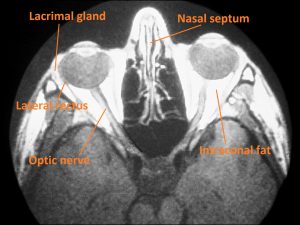
1.03 Axial CT of the right and left orbit.
- Pear shaped cavity housing the globe, nerves, vessels, lacrimal gland, extraocular muscles, tendons, trochlea, fat, and connective tissues
- Three major areas
- Intraconal space -within the muscle cone and intramuscular septae, and contains the globe, blood vessels, optic nerve, and the ciliary ganglion
- Extraconal -space outside the muscle cone that extends to the periosteum and contains the lacrimal gland and orbital fat lobules with septae
- Subperiosteal –potential space just deep to the periosteum
- Major structures
- Bordered by seven cranial bones
- sphenoid
- frontal
- zygomatic
- ethmoid
- lacrimal
- maxilla
- palatine
- Lacrimal gland and lacrimal drainage system
- Eccrine gland located extraconally in the anterior, superior, temporal quadrant of the orbit
- Order of drainage: lacrimal papilla → lacrimal puncta → canaliculi → common canalicular → lacrimal sac→ nasolacrimal duct
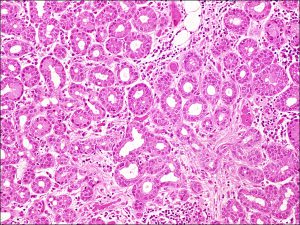
- Morphology appears similar to a cluster of grapes on a vine
- Groups of small circularacini that empty into a central lumen
- Acini and ducts are lined with secretory cuboidal epithelium containing eosinophilic granules and are surrounded by flat myoepithelial cells which help contract the acini
- Epithelial lining transitions from stratified squamous nonkeratinized at the punctual opening, to cuboidal in the lacrimal sac, and columnar in the nasolacrimal duct.
- It is common to see clusters of lymphocytes within the gland
- Bordered by seven cranial bones
1.04 Normal lacrimal gland
-
- Orbital septum-Fuses with the levator muscle/tarsus and forms the anterior border of the orbit
- Extraocular muscles –4 recti and 2 oblique
- Muller Muscle
- Smooth muscle running under the levator palpebreae superioris
- Sympathetic innervation affected in Horner’s syndrome
Eyelid
Mamalis Normal Eye
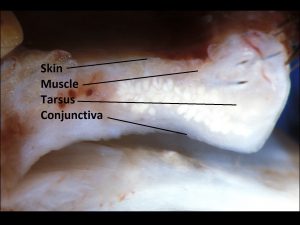
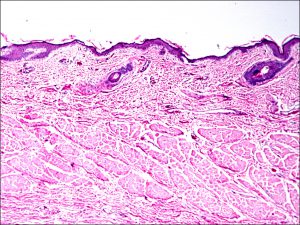
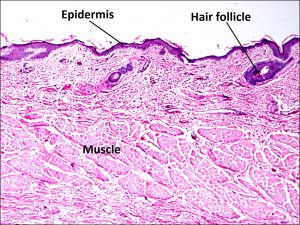
1.05 Gross cross-section of eyelid
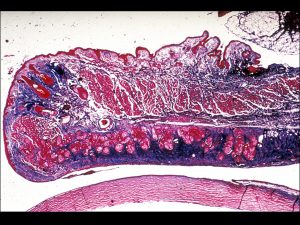
1.06 Trichrome stain of eyelid cross-section
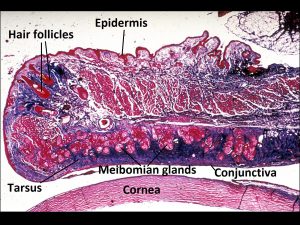
1.07 H&E stain of eyelid
1.08 Tarsus and meibomian glands
- Structure and cells present
- Form is provided by four layers of tissue
- Skin –keratinized stratified squamous epithelium
- Melanocytes and antigen presenting Langerhans cells may also be present
- No true dermis, so no rete ridges or pegs but does have some components of normal dermis
- Small hairs
- Eccrine glands
- Apocrine glands of Moll
- Sebaceous glands of Zeiss
- Muscle –orbicularis oculi, which can be broken into pretarsal, preseptal, and orbital parts
- Tarsus –Dense connective tissue without cartilage.
- Contains meibomian glands and accessory lacrimal gland of Wolfring.
- Ciliary muscle of Riolan (an extension of orbicularis) lies at the distal end of the eyelid
- Conjunctiva –Palpebral conjunctiva
- All three general types of glands are present in the eyelid
- Eccrine –Secretes via exocytosis
- Appears as described for the lacrimal gland
- Looks similar to grapes on a vine
- Cuboidal secretory cells with eosinophilic cytoplasmic granules form clusters of acini which empty into a central lumen
- Accessory Lacrimal Gland of Krauss –Located in fornices and empties into the fornix
- Accessory Lacrimal Gland of Wolfring –Located near superior border of tarsus and at the inferior border in smaller numbers
- Nick’s Tip: Imagine a “ring” of lacrimal glands around the palpebral fissure
- Appears as described for the lacrimal gland
- Apocrine –secrete oils by pinching off apical portions of the cell
- Apocrine glands have projections into the lumen due to their mechanism of release
- Glands of Moll –secrete oil onto hair cell at the lid margin
- Nick’s Tip: Remember Glands of “Mole” because the apocrine projections look like snouts and moles have snouts.
- Holocrine –sebaceous glands that secrete through release and breakup of the entire (whole) cell
- Appear empty due to dissolved secretions from tissue processingwith a central nucleus and foamy cytoplasm
- Differs from adipocytes,which have a flattened eccentric nucleus
- Sebaceous glands of Zeiss –sebaceous glands associated with eyelash hairs
- Meibomian glands –located in the tarsus, secretes oily layer of the tear film at the gray line of the lid margin
- Appear empty due to dissolved secretions from tissue processingwith a central nucleus and foamy cytoplasm
- Eccrine –Secretes via exocytosis
- Skin –keratinized stratified squamous epithelium
- Form is provided by four layers of tissue
Tear Film
- Covers the exposed cornea and globe,allows diffusion of various substances, and contains immunoglobulins, lysozyme, and lactoferrin
- 3 Layers
- Outer lipid layer –from meibomian glands, prevents evaporation
- Middle aqueous layer –from main and accessory lacrimal glands, provides moisture
- Inner mucin layer –from conjunctival goblet cells, prevents tear layer from breaking up, making the conjunctiva more “wettable”
Conjunctiva
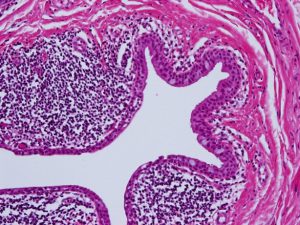
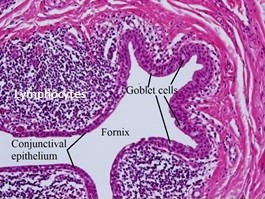
1.09 Low Magnification view of conjunctiva
1.10 Medium magnification view of forniceal conjunctiva
1.11 Higher magnification view of forniceal conjunctiva
- 2 to 5 cell thick mucous membrane
- Regions
- Palpebral
- Covers inner lid surface.
- Appears thin and tightly adhered to the tarsus
- Forniceal
- Conjunctiva reflects on self at cul-de-sac and attaches to globe
- Contains more goblet cells
- Lymphocyte patches similar to Peyer’s patches of the intestine are mostly T suppressor cells
- Bulbar -Fuses with tenon capsule and inserts into limbus
- Limbus region
- Caruncle –modified conjunctiva with hair follicles and sebaceous glands
- Nick’s Tip: Conjunctiva with hair follicles, sebaceous glands, and goblet cells is likely from the caruncle
- Palpebral
- Identification via cells and structure
- Two layers
- Nonkeratinizing squamous epithelial cells
- Thin, vascular substantia propria
- Lymph vessels
- Plasma cells
- Macrophages
- Mast cells
- Goblet cells -Useful in identifying the conjunctiva,more numerous as you move farther from the limbus.
- Two layers
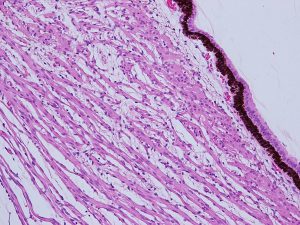
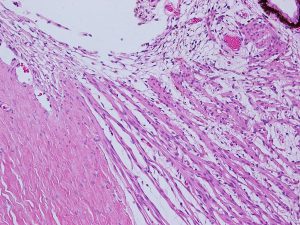
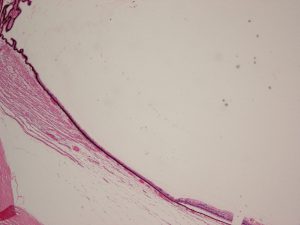
Sclera
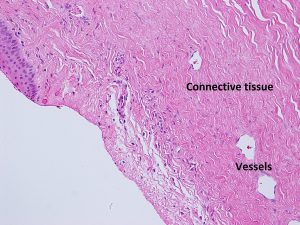
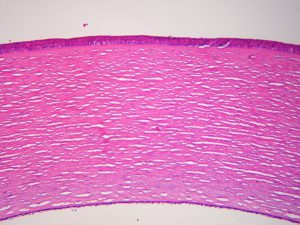
1.12 Transition from limbus to sclera
1.13 Normal Sclera
- Dense regular connective tissue covering 4/5 of the globe that is continuous with the corneal limbus anteriorly and the optic nerve sheath dura posteriorly
- Openings for cornea and optic nerve
- Thinnest (around 0.3 mm) behind insertion of rectus muscle tendons
- Mostly avascular with few exceptions -Superficial vessels of episcleral, intrascleral plexus posterior to limbus, and many emissaria containing arteries, veins, and nerves pass through the sclera
- Composed of three layers -episclera, stroma, and lamina fusca
- Anterior episclera
- Thin fibrovascular covering of the sclera between the more superficial tenon capsule and conjunctiva and the deeper superficial sclera
- Composed of a vascular plexus and loosely arranged collagen fibers
- Stroma
- Composed of type I collagen bundles, fibroblasts, and ground substance
- Emissarial channels are present and allow passage of nerves and blood vessels through the globe wall
- Entrance and exit of emissary vessels are the weakest points of the sclera, which is important in the extension of uveal melanomas
- Inner layer (lamina fusca)
- Fibroblasts, collagen fibers,and melanocytes
- Merges with subarachoidal and supraciliary lamellae of uveal tract
- Anterior episclera
- Opaque, in contrast to the cornea,for a number of reasons
- More variation in fibril diameter and separation
- More fibril interweaving into the sclera
- Vascular elements, such as emissaria
Cornea
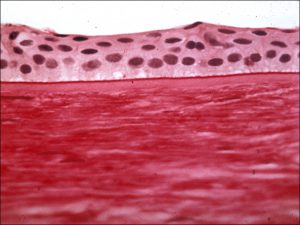
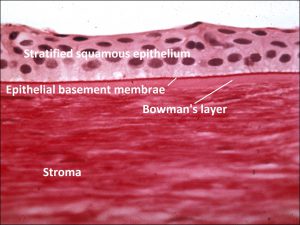
1.14 Normal Cornea
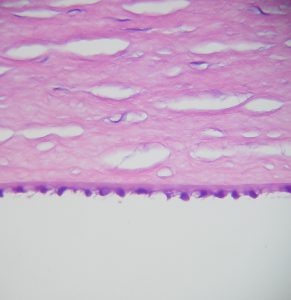
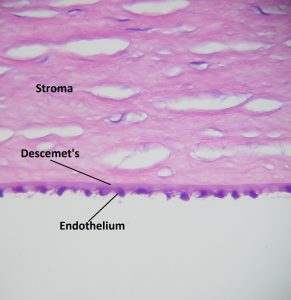
1.15 PAS Stained Cornea
1.16 Magnified Cornea
- Dimensions
- Diameter: 11-12mm horizontally and 9-11mm vertically
- Thickness: About 550 microns centrally to 650 microns peripherally
- Identification via cells and structure
- 5 Layers
- Epithelium –5-7 cells thick
- Non-keratinized, stratified squamous cells attached to basement membrane
- Histiocytes, macrophages, lymphocytes, Langerhans cells, and pigmented melanocytes may be present peripherally
- Bowman’s Layer –8-14 micronsthick
- Cellular collagen
- Modified layer of anterior stroma
- Not a true basement membrane, therefore does not stain with PAS
- Stroma –90% of cornea thickness
- Collagen lamellae
- Oblique in anterior third of stroma and parallel in posterior two thirds
- Uniform size and shape of fibrils contribute to transparency
- Ground substance
- Proteoglycans coats collagen fibrils for correct spacing
- Glycosaminoglycans can absorb water and cause stromal swelling
- Keratocytes
- Located between corneal lamellae
- Flat and evenly layered
- Contain many mitochondria, rough ER, and golgi apparatuses
- Create collagen and proteoglycans
- Collagen lamellae
- Descemet’s Membrane
- Basal lamina produced by the corneal endothelium
- 3-4 microns thick at birth, increases to 10-12 microns in adults
- Is a true basement membrane, so Periodic acid Schiff (PAS) positive
- Anterior banded zone and posterior non-banded zone
- Endothelium / Endothelial cells –
- Hexagonal-shaped cells in amonolayer
- Large nuclei and rich in mitochondria when young
- Cells decrease in number and grow in size with age and disease
- Relatively tight junctions between cells
- Actively transport ions
- Draws water out from stroma
- Maintains clarity of cornea
- Produces posterior portion of descemet’s membrane
- Epithelium –5-7 cells thick
- 5 Layers
Trabecular Meshwork
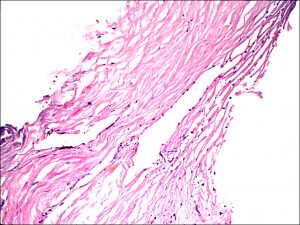
1.17 Trabecular Meshwork
Normal trabecular meshwork. Schwabes line is seen at the termination of descemets membrane. Also seen is the nonpigmented trabecular meshwork, the pigmented area, and the scleral spur.
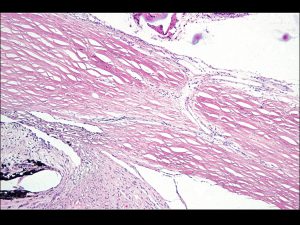
1.18 Normal trabecular meshwork
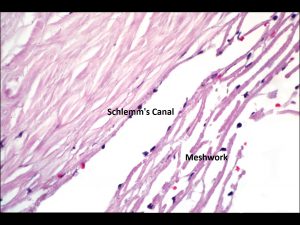
1.19 High magnification view of schlems canal and juxtacanalicular tissue.
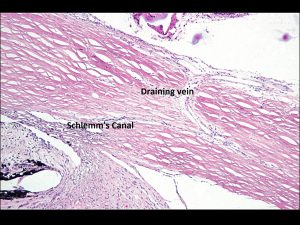
1.20 Schlemms canal with a draining aqueous vein
- Meshwork is comprised of tissue derived from the cornea, sclera, iris, and ciliary body that sits on a ledge formed by the scleral spur and stretches from Schwalbe line anteriorly to the scleral spur and ciliary body posteriorly and drains aqueous fluid to the Schlemm canal
- Structure and cells of the trabecular meshwork
- Three layers from inner to outer
- Uveal –Cords of trabeculae beams lined by trabeculocytes form a meshwork that is less elastic than the coneoscleral’s
- Corneoscleral meshwork -A laminar pattern of thin, flat, and perforated sheets of tissue lined by trabeculocytes
- Juxtacanalicular tissue -Endothelial meshwork of cells located between the corneoscleral mesh and Schlemm canal.
- Narrow path with proteoglycans and glycoproteins can cause resistance to outflow
- Trabeculocytesform a monolayer lining of the beams and sheets that form the uveal and coneoscleral meshwork
- Contractile and phagocytic
- Usually contain pigment granules
- Basal lamina forms the exterior of beams and collagen and elastic fibers create the inner core
- Increasing pigmentation, thickening of the basement membrane, and a decrease in number occurs with age
- Three layers from inner to outer
- Schlemm canal
- Continuous monolayer of nonfenestrated endothelium with thin connective tissue wall
- Endothelium basement membrane can be difficult to identify
- Endothelial cells contain micropinocytotic vesicles at their apical and basal surfaces
- Large vesicles with a single membrane lining may be seen at the internal canal wall
- 25-30 collector channels
- Drain from Schlemm canal to the deep and midscleral venous plexuses.
- A minority drain to the episcleral plexus as aqueous veins, which may be visible in the conjunctiva under the slit lamp
- Continuous monolayer of nonfenestrated endothelium with thin connective tissue wall
Iris
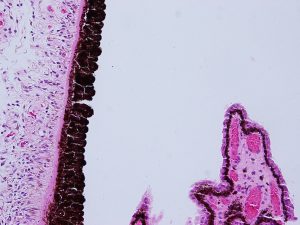
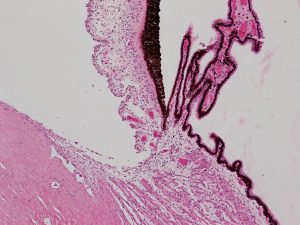
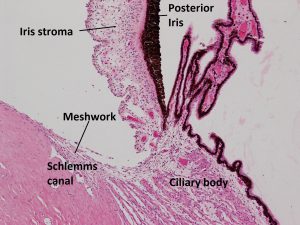
1.21 Angle with trabecular meshwork, iris, and ciliary body
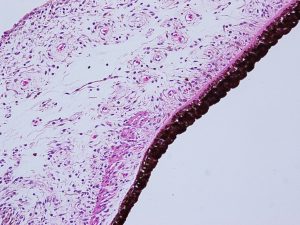
1.22 Posterior iris with portion of ciliary body
1.23 Iris stroma
- The most anterior part of uvea, separating the anterior segment into anterior and posterior chambers
- Made up of five layers composed of muscle, blood vessels, connective tissue, pigment cells, and melanocytes .
- Anterior border layer –condensation or iris stroma and melanocytes
- Stroma–contains melanocytes, blood vessels, nerves, fibrocytes, and clump cells in a hyaluronic acid containing matrix with collagen fibrils
- Melanocytes –number and size of pigment made bythese cells determines iris color
- Clump cells
- Type I: Macrophages, clump cells of Koganei
- Type II: Smooth muscle cells
- Vessels
- Formed from nonfenestrated endothelial cells
- Contain hyaline and stain eosinophilic
- Surrounded by basement membrane with associated pericytes and collagen fibrils, appearing thick walled
- No internal elastic lamina present in the intima
- Compose majority of the iris stroma, but the anterior border is usually avascular
- Nerves
- Myelinated and nonmyelinated fibers
- Sensory, vasomotor, and muscular functions in the stroma
- Covered by patchy connective tissue, which connects into ciliary body
- Muscular layer
- Sphincter muscle
- Smooth muscle fibers are located in the deep stroma, anterior to the pigment epithelium near the pupillary margin.
- Mostly parasympathetic innervation
- From CN III nucleus
- Starts at Edinger-Westphal nucleus and travels with the inferior part of CN III through the cavernous sinus to the inferior oblique and then go on to synapse at the ciliary ganglion
- Postganglionic fibers follow the short ciliary nerves to the sphincter
- Notable among postganglionic autonomics for myelination
- Muscarinic stimulation used pharmacologically
- Sympathetic innervation may be inhibitory
- From CN III nucleus
- Dilator muscle
- Formed from smooth muscle cells with myofilaments and melanosomes, it lies anterior to the posterior pigmented layer
- Sympathetic and parasympathetic innervation
- Normal contraction of dilator with alpha 1 stimulation
- First order neuron from Ipsilateral posterolateral hypothalamus synapses in spinal cord around level T1.
- Second order preganglionic neuron exits cord, goes over lung apex, through the stellate ganglion, and then synapses at superior cervical ganglion
- Third order postganglionic neuron enters the internal carotid plexus, then cavernous sinus, and then courses with the ophthalmic division of CN V to the dilator muscle
- Cholinergics may inhibit contraction
- Normal contraction of dilator with alpha 1 stimulation
- Sphincter muscle
- Anterior pigment epithelium–Cell bodies give rise to the dilator muscle
- Posterior pigment epithelium–Continuous with the ciliary body and curling around pupil to create the pigment ruff, these densely pigmented polar cells’ basal surface borders the posterior chamber
Ciliary Body
1.24 Angle with trabecular meshwork, iris, and ciliary body
1.25 Iris and portion of ciliary body
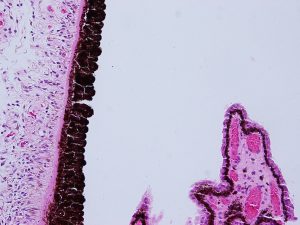
1.26 Pars plicata
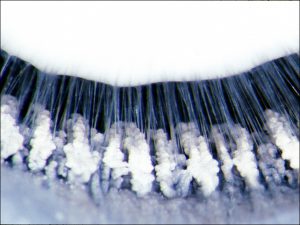
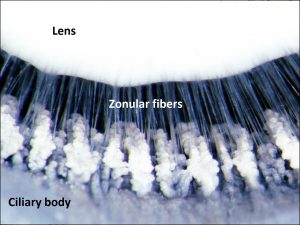
1.27 Zonules attached to ciliary processes
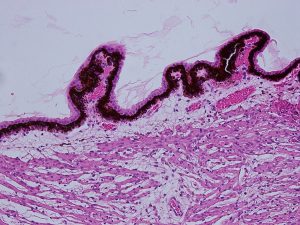
1.28 Pars plana
1.29 Ciliary muscle
1.30 Pars plana transitioning to retina at ora serrata
- Located between the anterior and posterior segments of the eye, this is the portion of the uvea responsible for aqueous humor production and lens accommodation
- Two parts
- Pars plicata
- Folded/plicated appearance is due highly vascular radial folds, or ciliary processes, each containing a capillary plexus where the rate of blood flow affects aqueous humor production and is altered by sphincter tone, smooth muscle innervation, and vasoactive substances
- Most of the zonular fibers attach to these ciliary folds
- Pars plana
- Smooth appearing and located immediately posterior to the ciliary processes and anterior to the ora serrata, about3-4 mm from the corneal limbus
- Connects the ora serrata and ciliary processes
- Pars plicata
- Two cell layers line the ciliary body
- Outer pigmented epithelium -Cuboidal cells whose basal lamina faces the iris and contain large nuclei, many mitochondria, a large endoplasmic reticulum, and multiple melanosomes
- Inner nonpigmented epithelium
- Appear cuboidal in the pars plana and more columnar in pars plicata, basal lamina faces the posterior chamber, also contain large nuclei and many mitochondria with occasional melanosomes present
- Stroma contents
- Fibroblasts
- Collagen fibrils
- Large fenestrated capillary complexes from the anterior and long posterior ciliary arteries
- Ciliary muscle-insert intothescleral spur and fibers of the trabecular meshwork, affecting outflow of aqueous humor
- Composed of smooth non-striated muscle fibers surrounded by basal lamina which form bundles covered by fibroblastic sheath instead of collagen
- Three layers
- Longitudinal outer layer (Muscle of Brucke)–makes up the majority of the ciliary muscle and attaches to the scleral spur, induced by pilocarpine to open the meshwork
- Oblique (radial)middle layer–attaches to the zonules for accommodation via zonular relaxation
- Circular (round or Muller’s) inner layer
- Nerve fibers may also be present throughout the muscle
- Myelinated and unmyelinated
- Mostly parasympathetic from short ciliary nerves of CN III
- Rare sympathetic fibers may be present as well
- Cholinergics contract the ciliary muscle
Choroid
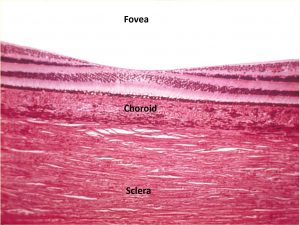
1.31 Normal choroid
1.32 Choroid starting at the ora serrata
- Pigmented and vascular tissue extending from the optic nerve to the ora serrata
- Forms the posterior part of the uveal tract and the middle coat of the posterior globe
- Blood flow supports the outer retina
- Supplied by the long and short posterior ciliary arteries and the perforating anterior ciliary arteries
- Drains to the vortex system
- Relatively high blood flow means oxygen content of venous blood is higher than elsewhere
- Three layers of vessels
- Inner choriocapillaris
- Plane of large, thin walled fenestrated capillaries
- Lies beneath the RPE
- Pericytes present along outer wall of capillaries
- Middle layer of small vessels
- Non fenestrated
- Outer layer of large vessels
- Non fenestrated
- Notable for presence of internal elastic lamina and media containing smooth muscle typically seen in small arteries
- Inner choriocapillaris
- Bruch Membrane
- Lamina stretching from the optic disc margin to the ora serrata
- Formed from fusion of the retinal pigment epithelium basal lamina and choriocapillaris
- PAS positive
- Five structural components(can think of these as a sandwich)
- Basement membrane of RPE(bread)
- Inner collagenous zone(meat)
- Thick elastic band(cheese)
- Outer collagenous zone (meat)
- Basement membraneof choriocapillaris (bread)
- Stroma
- Numerous melanocytes are present, in contrast to the RPE
- Also contains rare macrophages, lymphocytes, mast cells, and plasma cells
- Nerve fibers and collagen fibers also located in the extracellular space
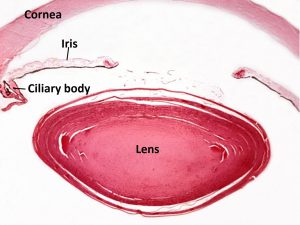
Lens
1.33 Normal Lens
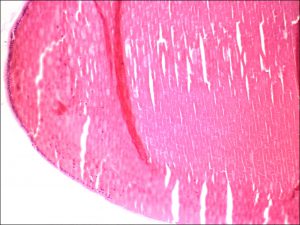
1.34 Magnified Lens (PAS stain)
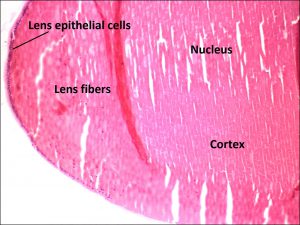
1.35 Equatorial lens
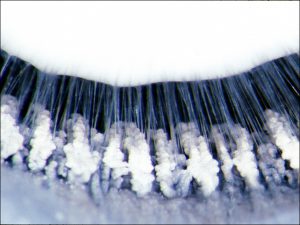
1.36 Normal cortical lens fibers
- Normally avascular, biconvex and responsible for about 1/3 of the eye’s refracting power
- Increases in lens size with age are accompanied by changesin curvature and refractive gradient
- Lack of innervation or vascular supply –relies on aqueous and vitreous
- Layers from outer to inner
- Lens capsule –Completely encloses the lens
- Formed from the basal lamina of lens epithelial cells
- Composed of type IV collagen, thickest anteriorly (about 15.5 microns) and thinnest posteriorly (about 2.8 microns)
- Lens epithelial cells –Single layer of cuboidal cells with prominent nuclei present only anterior to the capsule’s equator
- Basal end lies against the lens capsule with the apex pointing into the lens
- Three regions
- Stable central zone decreases with age
- Intermediate zone has rare mitosis
- Preequatorial cuboidal cells form a germinative zone responsible for continued growth of the lens through life and may proliferate and cause PCO after phacoemusification if left behind.
- Cortex and nucleus
- Made from fiber cells, the inner nucleus is formed at birth, and outer cortex is created as new fibers are added
- Made of spindle shaped lens fibers formed from epithelial cells that lose their nucleus and most organelles
- Lens capsule –Completely encloses the lens
1.37 Zonules
- Zonular fibers (suspensory ligaments)
- Composed of multiple filaments of fibrillin that originate from the basal lamina of nonpigmented epithelial cells of the pars plana and pars plicata of the ciliary body
- Attach to the anterior and posterior to the capsule equator
- Under tension for distance vision and more relaxed for accommodation
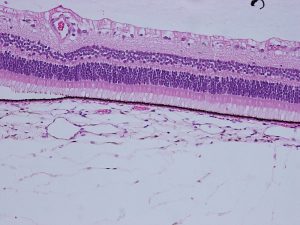
Retina
Composed of inner neurosensory retina and outer retinal pigment epithelium (RPE)
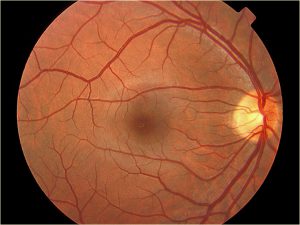
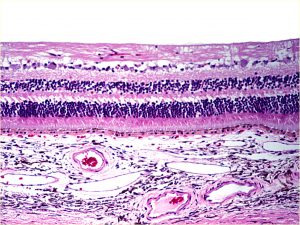
1.38 Normal Retina –macula is between arcades
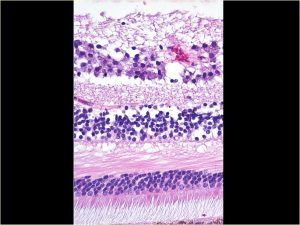
1.39 Retina –ganglion cell layer is only 1 cell thick in most areas of the retina
1.40 Layers of retinain macula –ganglion cell layer has multiple layers
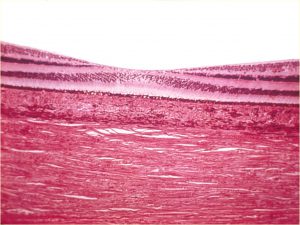
1.41 Fovea
Layers (from innermost to outermost)
-
- Internal limiting membrane –not a true basement membrane, formed from Müller cell footplates and attachments to the basal lamina
- Basal lamina appears smooth on vitreal side but wavy on retinal side as it follows along Müller cells
- Nerve fiber layer –formed from ganglion cell axons
- Ganglion cell layer -contains ganglion cell bodies near the inner surface of the retina
- Inner plexiform layer –contains bipolar and amacrine cell axons, ganglion cell dendrites, and synapses
- Inner nuclear layer –Location of bipolar, Müller, horizontal, and amacrine cell nuclei
- Middle limiting membrane
- Outer plexiform layer –Formed from connections between photoreceptor synaptic bodies and horizontal and bipolar cells, it’s also known as the Henle fiber layer at the macula, where it’s thickest.
- Outer nuclear layer
- External limiting membrane –highly fenestrated and located next to the RPE, this is not a true membrane, but formed from attachments of photoreceptors and Müller cells
- Photoreceptors -rod and cone inner and outer segments
- RPE
- Bruch’s Membrane
- Inner basement membrane of RPE
- Collagen layer
- Middle elastic layer
- Collagen layer
- Outer basement membrane of choroid (choriocapillaris)
- Choroid
- Sclera
- Internal limiting membrane –not a true basement membrane, formed from Müller cell footplates and attachments to the basal lamina
- Neurosensory Retina-Three major elements
- Neuronal portion
- Neuroepithelial rod and cone cells in contact with apical part of RPE
- Rod photoreceptors
- Outer segment includes a central cilium and multiple discs unattached to the cell membrane, in contrast to cones
- Inner segment has an outer portion with ellipsoids storing many mitochondria and inner portion containing glycogen storing myoids and a synaptic body, or spherule
- Cone photoreceptors
- Outer structureis similar to rods but discs are attached to the cell membrane
- Inner structure has a more complex synaptic body, or pedicle, than the rod’s, which interacts with other photoreceptors as well as horizontal and bipolar cell structures
- Rod photoreceptors
- Horizontal cells with processes that synapse with photoreceptors and pass horizontally through the outer plexiform layer
- Amacrine cells
- Inner segment
- Outer segment in contact with the RPE apices
- Bipolar cells are vertically oriented
- Dendrites synapse with photoreceptors
- Axons synapse with ganglion and amacrine cells of the inner plexiform layer
- Dendrites synapse with photoreceptors
- Ganglion cells
- Axons bend to form the nerve fiber layer and then the optic nerve
- Neuroepithelial rod and cone cells in contact with apical part of RPE
- Glial portion
- Müller cells
- Vertically oriented glial cells stretching from the external limiting membrane to the internal limiting membrane
- Provide structural and nutritional support to the retina
- Nuclei are located within an inner nuclear layer
- Other cells providing support
- Astrocytes
- Microglia
- Müller cells
- Vascular portion
- A single layer of nonfenestrated endothelial cells form the vessels
- Cells are covered by a basal lamina and have tight junctions to support the inner blood-retina barrier
- Vessels are notable because they lack an internal elastic lamina and feature sporadically appearing smooth muscle rather than the continuous layer seen in most vessels
- Pericytes or mural cells are present sporadically in the vessel’s basement membrane and attach to the endothelial basal lamina
- Areas of perfusion
- Central retinal artery branches perfuse the inner part of the retina to the Outer Nuclear Layer
- Cilioretinal artery may rarely supply the macula
- A single layer of nonfenestrated endothelial cells form the vessels
- Neuronal portion
- Retinal Pigment Epithelium-the outer pigmented epithelial layer of the retina extending from the optic disc to merge with the ciliary body’s pigmented epithelium
- Functions
- Metabolic -vitamin A metabolism, transport of materials into and out of the RPE, and phagocytosis of photoreceptor outer segments
- Structural -creation of the Bruch membrane basal lamina, mucopolysaccharide matrix surrounding the outer segments, and maintenance of the outer blood-retina barrier
- Vision –provides light absorption, scatter reduction, and heat exchange
- Composed of a monolayer of hexagonal shaped epithelial cells
- Cells are polar
- Numerous folds on the basal side attach to a thin basal lamina to form the inner layer of the Bruch membrane
- Apically, numerous villous processes interact with the outer segments of photoreceptors
- Cells vary in appearance by location
- Foveal cells are relatively tall and thin with more melanosomes
- Peripherally, cells are shorter, broader, and less pigmented
- Likely corresponds with higher metabolism in the more active fovea
- Cells cytoplasm contents
- Melanosomes appear as numerous round/ovoid pigment granules
- Membrane-enclosed phagosomes containing the engulfed contents of disc outer segments
- Lipofuscin granules, or “wear and tear” pigment, likely arising from remnants of photoreceptor disc phagocytic activity, increases with age and may be visible histologically
- Large round nucleus
- Many mitochondria, rough endoplasmic reticulum, and Golgi apparatus
- Cells are polar
- Functions
- Notable Structures
- Macula -located between temporal vascular arcades, 5 to 6 mm in diameter, and identified histologically by the presence of more than one layer of ganglion cell nuclei
- Fovea -depression at the center of the macula measuring about 1.5 mm in diameter with numerous cones for color vision and visual acuity
- Foveola–term for the central depression where the photoreceptor layer is comprised of only densely packed cones
- Photoreceptor cells in this region bend towards the internal limiting membrane to form the fovea externa
- Photoreceptors, Müller cells, and other glial cells are normally the only cells present though ganglion cell nuclei may rarely be found beneath the ILM
- Foveal avascular zone –similar location to foveola. Not always truly avascular
- Parafovea –surrounds the fovea and is the area where the ganglion cell layer, inner nuclear layer, and outer plexiform layer are thickest
- Perifovea -outermost region of the macula
- Foveola–term for the central depression where the photoreceptor layer is comprised of only densely packed cones
- Ora Serrata-the peripheral junction of the retina and pars plana
- Lies about 6.5 mm temporally and 5.75 mm nasally from the Schwalbe line.
- Temporal portion appears relatively smooth compared to more serrated nasal side
- Located within a watershed zone between the anterior and posterior vascular systems formed as retinal vessels end in loops before entering
- Histologically, the peripheral retina of this area often contains malformed photoreceptor cells and commonly appears cystic in paraffin sections (Blessig-Iwanoff cysts)
Optic Nerve
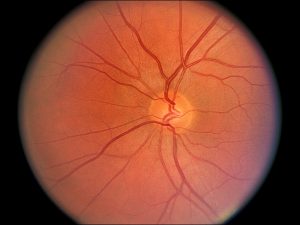
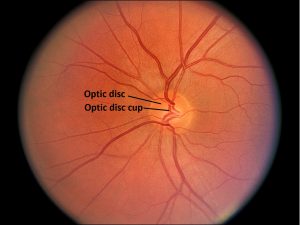
1.42 Fundus photo of normal optic nerve
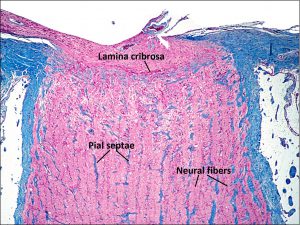
- Formed as axons from the ganglion cell layer of the retina exit through the lamina cribosa, a mesh like areaof the sclera.
- Axons are unmyelinated until the pass through the lamina cribosa
- Myelinated by oligodendrocytes after passing the lamina cribosa
- Fascicles are wrapped pial septae and the entire structure is covered in dura mater sheath
- Nicks Tip: After passing through the lamina cribosa, the nerve may be thought of as a fiber-optic cable
- Individual myelinated axons are analogous to optical fibers coated in plastic
- Fascicles of axons wrapped in pial septae is similar to bundles of optical fibers wrapped in protective casing
- Entire nerve is encased in protective sheath of dura mater like a fiber optic cable is with steel
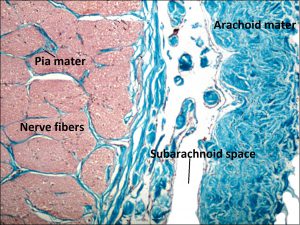
- Layers from outer to inner
- Dura mater–optic nerve sheath, continuous with the posterior sclera
- Arachnoid mater–comprised of meningothelial cells, provides the nerve’s blood supply
- Subarachnoid space–contains CSF, continuous with subarachnoid space of the brain
- Pia mater–Pia’s septae wrap around nerve fiber bundles, growing into the parenchyma
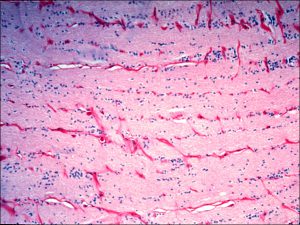
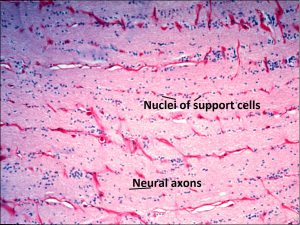
- Nerve fibers
- Neurons’ nuclei are located in the ganglion cell layer of the retina
- Support cells –Astrocytes, oligodendrocytes, microglial cells
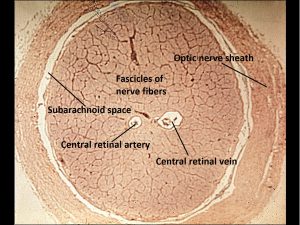
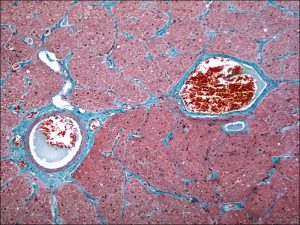
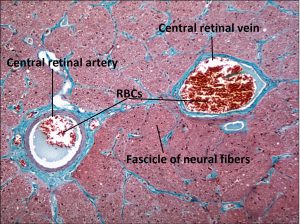
- Central retinal artery and vein
- Artery and vein share a common adventitial sheath
- Artery is usually nasal to the vein
- Artery and vein get closer to each other as they get closer to entering the eye
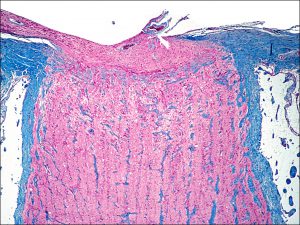
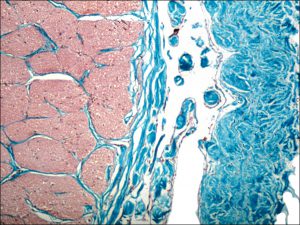
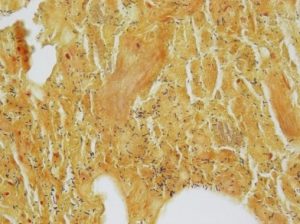
1.43 Trichrome stain optic nerve
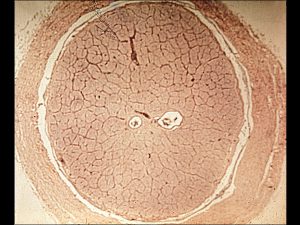
1.44 Cross-section of optic nerve
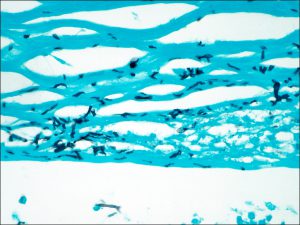
1.45 Optic Nerve Sheath
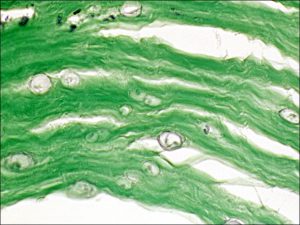
1.46 Support cellsof the optic nerve
1.47 Central Retinal Artery & Vein
Classification of disorders:
Building on a knowledge of the normal cellular structure and contents of the eye, diagnosis of ocular disease begins with classifying the type of pathology into one of 5 types –congenital, inflammation, degenerationand dystrophy,neoplastic, or infectious
Congenital
- An abnormality in tissue size, location, organization, or amount
- Choristoma–Otherwise normal tissue in an abnormal location, e.g. a dermoid
- Hamartoma-Abnormal growth of tissue through hyperplasia or hypertrophy in a normal location, e.g. a cavernous hemangioma
- Teratoma–A tumor composed of all three embryonic germ layers
- Congenital/genetic-Inborn
Inflammation
- Broadly classified as acuteversus chronic and localized versus diffusedisease with various celltypes typical to each class (individual cells are described further in cellular histopathology chapter)
- Acute inflammation–Typically involvespolymorphonuclear leukocytes (PMNs), such as neutrophils, eosinophils, and basophils, though these may also be seen in chronic inflammation
- Chronic inflammation –Can be further broken into granulomatous and nongranulomatous inflammation
- Lymphocytes and monocytes (such as histiocytes or macrophages) are common to both chronic granulomatous and nongranulomatous disease
- Granulomatous inflammationis recognized by the presence of granulomas and multinucleated giant cells formed from epithelioid histiocytes
- Granulomas -aggregates of epithelioidhistiocytes.
- Multinucleated giant cells, such as Langhans cells, Touton giant cells, or foreign body giant cells, formed from merging of epithelioidhistiocytes are common
- Caseating granulomas have a necrotic center, in contrast to the intact cells seen in noncaseating granulomas
Degeneration and dystrophy
- Degeneration -Wide variety of pathologic changes usually involving loss of tissue mass or accumulation of acellular tissue that isacquired over time, often in association with some general disease, e.g. lens calcification associated with congenital cataracts
- Dystrophy –An inherited condition, usually bilateral and symmetric
Neoplastic
- Abnormal growth of some tissue type classified as benign or malignant, though some share features of both classes and may be referred to as intermediate or borderline growths.
- General features of malignant neoplasms
- Nuclear hyperchromasia
- Pleomorphism
- Necrosis
- Hemorrhage
- Mitotic activity
- Classification of neoplasm by tissue type
- Epithelium –growth pattern usually involves tubules or cords
- Benign –Hyperplasiain general epithelium and adenomain glandular tissue
- Malignant –carcinomain general epitheliumand adenocarcinomain glandular tissue
- Connective or soft tissue –growth is usually flat sheets of tissue
- Benign –structure + “oma”
- Malignant –structure + “sarcoma”
- Hematopoietic –usually loosely arranged pattern
- Benign –Hyperplasiaor infiltrate
- Malignant –Leukemiaor lymphoma
- Epithelium –growth pattern usually involves tubules or cords
Infectious
- Various bacteria, viruses, fungi, and parasites are able to infect and damage ocular tissues. Individual pathogens, associated diseases, and histological appearances are discussed in further detail within the immunology chapter.
- Bacteria –can be classified by stain (presence of peptidoglycan wallwith gram stain, Ziehl-Neelsen stain for acid-fast), shape (cocci, bacilli, or coccobacilli), metabolic activity (aerobic, anaerobic), and enzymatic activity (catalase, oxidase, urease, lactase, etc.)
1.48 Gram positive bacteria
- Fungi –multicellular pathogen seen in infections of several ocular tissues that stains silver with GMS stain
1.49 GMS stain of yeast
- Viruses –a number of viruses are associated with various pathologies in the eye with some listed in various chapters of this guide. There is not aspecific histopathologic stain for viruses as there are for bacteria, fungi, and acanthamoeba
- Parasites
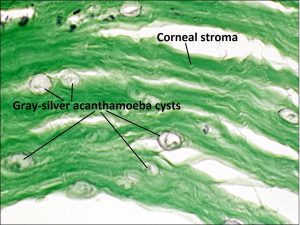
- Though a number of parasites may infect the eye, acanthamoeba is most commonly seen and cysts are best visualized with the Gridley stain
1.50 Gridley stain showing Acanthamoeba cysts in the cornea
References:
Yanoff M, Fine BS. Ocular Pathology, A Text and Atlas. Lippincott Williams & Wilkins; 1989.
American Academy of Ophthalmology. (2016).Basic and clinical science course. San Francisco, CA.